Choosing the Right C-Arm: Comparing Today’s Top Veterinary Models
Choosing a C-arm is one of the most significant equipment decisions a veterinary practice can make.
Between mobile and mini systems, varying dose technologies, and wildly different footprints, it can feel overwhelming to determine what actually matters for your clinical needs.
Whether your practice focuses on orthopedics, ER, general surgery, or mobile specialty work, the right C-arm will strike the perfect balance between image quality, ease of use, safety, and cost.
This guide breaks down the key differences and highlights what to look for.
Mobile vs. Mini C-Arms: Which One Fits Your Practice?
Mobile C-Arms
These full-size systems are best suited for:
High-volume orthopedic hospitals
Specialty centers performing complex soft tissue or vascular interventions
Clinics with spacious ORs and high caseloads
Advantages and Considerations:
Full-size mobile C-arms offer a larger field of view and greater versatility for advanced interventional work, often with features such as DSA. However, they come with clear trade-offs—a larger footprint, higher cost, and greater space and training requirements to integrate smoothly into a practice.
Mini C-Arms
Initially designed for human extremity imaging, veterinary-focused mini C-arms have evolved into highly effective tools for small-animal orthopedics and foreign-body procedures.
A strong example is the Orthoscan Tau 1515, which features a compact, all-in-one footprint that fits seamlessly into ORs that were not originally planned to support fluoroscopy.
Advantages and Considerations:
Mini C-arms are highly maneuverable and cost-effective, making them ideal for general practices, ortho-focused GPs, and mobile surgeons who need a small footprint and easy mobility. Their compact size does come with limitations, including a smaller field of view, limited full-body imaging, and the potential absence of advanced features such as DSA—Flat-Panel Detectors vs. Image Intensifiers.
Flat-Panel Detectors (FPDs)
FPDs are now considered the gold standard due to:
Higher resolution
Lower noise
Better consistency over time
Reduced distortion
Many modern C-arms use CMOS flat-panel technology, which delivers sharp, bright images with enhanced detective quantum efficiency to reduce noise and improve image quality at lower doses
Image Intensifiers
Image intensifiers are an older technology. While functional and often cheaper (especially refurbished), they:
Degrade over time
Produce more distortion at the edges
Offer lower contrast and resolution
For practices focused on orthopedic precision, flat-panel detectors are usually worth the upgrade.
Image Resolution and Dose: What Truly Matters
Resolution
Look for systems that offer:
High pixel density
High signal-to-noise ratio
Clear visualization of fine bone detail
Dose Reduction
Radiation safety is a critical consideration for veterinary teams. Modern systems use a combination of hardware and software to reduce dose.
Digital Subtraction Angiography
DSA or Digital Subtraction Angiography is most relevant for:
Vascular studies
Shunt evaluations
Pacemaker lead assessment
While not every C-arm includes DSA, practices planning to expand into advanced soft-tissue or cardiac procedures may want to prioritize it.
Footprint, Maneuverability, and OR Workflow
Clinics with limited space, or those that move between multiple Ors, should focus heavily on footprint and ease of movement.
If your OR space is tight or you anticipate moving between rooms, a mini C-arm may significantly improve workflow without sacrificing clarity.
What Does “Value” Look Like for Your Type of Practice?
For general practices, value often comes from cost-effective imaging, a small footprint, and easy day-to-day use. At the same time, orthopedic-focused GPs tend to prioritize high-resolution images, low dose, and workflow efficiency. This makes a flat-panel mini C-arm an excellent fit, especially for clinics performing frequent TPLOs where a newer detector pays off quickly.
Emergency and critical care hospitals benefit most from speed, reliability, and the ability to guide foreign body retrieval or urgent orthopedic stabilization, and may choose either a mobile or mini system depending on their caseload.
Specialty hospitals usually require full capabilities, including a large field of view, advanced software, and often DSA, making a full-size mobile fluoroscopy unit the most appropriate choice.
Meanwhile, mobile surgeons see the highest ROI from compact, portable, durable systems—typically mini C-arms designed with veterinary-first software and rugged construction for use across multiple clinics.
What Actually Matters?
When choosing a C-arm, the most important considerations are:
Does it deliver the image quality you need for your caseload?
Can your team use it quickly and confidently?
Does the footprint fit your clinic’s workflow?
Will the dose profile keep your team safe?
Is the price aligned with the value and procedures you plan to offer?
In the end, choosing the right C-arm is about finding the balance that fits your practice: image quality that supports the procedures you perform, technology your team can use confidently, and a system that integrates smoothly into your physical space and workflow.
Whether you’re upgrading your orthopedic capabilities, expanding your ER tools, or simply looking to improve surgical precision, the right C-arm can elevate the standard of care you deliver every day.
Comparing the Mindray Vetus E5 vs. the GE Sound-Antech LOGIQ e Vet
A real-world comparison for busy practices
Whether you’re upgrading your ultrasound capabilities or balancing performance with budget, the Mindray Vetus E5 and the GE Sound-Antech LOGIQ e Vet are two machines that frequently come up in conversation.
Both aim to help you scan confidently, efficiently, and with diagnostic clarity — but they take different paths to get there.
Let’s break down their differences and see which might be the best fit for you and your team.
1. Workflow & User Experience
Designed specifically for veterinary workflow, the E5 centers on intuitive, animal-centric scanning:
Touch-sensitive gain and controls make adjustments quick, even in dim exam rooms.
iTouch one-click optimization simplifies on-the-fly improvements in image quality.
Veterinary presets and iWorks protocols mean less time tweaking settings and more time scanning.
iReport templates support rapid, polished reporting without external software.
The overall feel is practical and vet-friendly — great for general practice, reproduction work, abdominal scans, and standard cardiac assessments.
GE LOGIQ e Vet
The LOGIQ e Vet carries forward GE’s tradition of hospital-grade imaging in a portable form:
Laptop-style portability with an HD screen and sealed controls for easier cleaning. The
Scan Assistant feature helps streamline exam routines.
Classic GE ergonomics, with optional trackpad/trackball navigation for seasoned sonographers.
If you’re used to traditional ultrasound interfaces or want a familiar platform across specialties, the LOGIQ e footprint will be comfortable and dependable.
2. Image Quality & Processing Tools
Mindray Vetus E5
Mindray’s ZST+ imaging platform powers the E5, giving you a suite of advanced image tools that matter in veterinary clinical work:
HR Flow & advanced Doppler modes support fine vascular assessment.
Natural Touch Elastography helps assess tissue stiffness (particularly in hepatic, splenic, and soft-tissue evaluations).
iClear speckle reduction and SmartCalc automated measurements shrink noise and speed quantification.
This suite of tools tends to improve everyday imaging quality, especially in small-animal abdominal work and soft-tissue characterization.
GE LOGIQ e Vet
LOGIQ e brings grayscale and Doppler imaging:
Broad imaging modes like B-mode, M-mode, Color Flow, Power Doppler, PW Doppler, and more are standard.
LOGIQ e’s core image engine is proven and reliable for abdominal, cardiac, and vascular imaging across species.
For practices with varied caseloads — from small animals to equine — the LOGIQ platform’s versatility is a key strength.
3. Portability & Durability
Lightweight and portable enough for in-clinic or off-site use, without a heavy cart.
Durable waterproof/dustproof control panel designed to tolerate hair, fluid, and accidental knocks — essential in high-volume vet settings.
Long battery life and easy probe switching keep daily workloads running smoothly.
GE LOGIQ e Vet
A laptop-style form factor makes it inherently portable, ideal for multi-room or field applications.
90-minute battery life between charges is standard on many configurations.
The E5’s design focuses on vet-specific ruggedness, while the LOGIQ e emphasizes proven portability and clinical durability.
4. Value & Warranty Considerations
Often, more aggressive pricing, including standard accessories like one transducer, cart, training, and a robust warranty.
With tools like SmartCalc and iReport included, practices find they get more built-in functionality per dollar.
GE LOGIQ e Vet
Carries a strong service and support ecosystem.
Pricing can be higher, especially when equipped with a full range of vetted veterinary probes and extended support plans.
5. Which One Fits Your Practice?
Here are a few quick scenarios:
General Practice:
The Vetus E5 often delivers excellent image quality, intuitive workflows, and substantial value. Its vet-centric software and reporting tools can save time in busy daily scanning.
Mixed Practice or Specialty Referral:
If you’re doing more cardiac or equine evals and want a platform with broad familiarity and flexibility, the LOGIQ e Vet might be a good choice.
Mobile / Field-Based Work:
Both units are portable, but Mindray’s rugged, purpose-built portability gives it a slight edge for rugged field use, while LOGIQ e’s laptop-style design and battery support make it ideal for point-to-point scanning.
The bottom line is that both systems have earned their place in modern veterinary practices. The E5 excels in intuitive vet workflows and built-in tools, while the LOGIQ e Vet brings a trusted, flexible platform with strong imaging fundamentals that spans diverse case loads.
The Mindray Vetus E5 stands out by delivering more practical performance for everyday veterinary work at a better overall value. Built specifically for veterinary workflows, it offers faster setup, one-click image optimization, cleaner abdominal and soft-tissue imaging, and built-in reporting that saves time on every scan.
Its rugged, vet-friendly design holds up in busy exam rooms, while advanced imaging tools come standard—without costly add-ons. For practices that want excellent image quality, efficiency, and ROI without paying a premium for a legacy platform, the Vetus E5 is the clear choice.
Affordable Vet Imaging with the Vetus E5 Ultrasound
If you’re looking to expand your diagnostic services while keeping budgets in check, then you’re in the right place. It’s the perfect time to take a closer look at the Vetus E5 ultrasound. This system bridges the gap between basic ultrasound units and premium machines, offering veterinary-specific features in a value-focused package.
Why Invest in an Ultrasound Now?
In today’s fast-paced veterinary environment, clients expect more, and it’s become a standard for practices to deliver high-quality diagnostics faster. Here are a few motives driving investment:
Broader diagnostic scope: With ultrasound, you can offer services such as soft-tissue evaluation, cardiac screening, reproductive imaging, abdominal scans, and more.
Improved case flow and retention: In-house scanning means fewer referrals, faster turnaround, and better client satisfaction.
Revenue diversification: Ultrasound opens up billable procedures and follow-ups. Even a modest increase in scan volume can pay off.
Upgrading your diagnostic tools is a strategic investment in your practice’s financial growth.
Meet the Vetus E5 — What It Offers
First, the question that’s always top of mind - price and support. We offer financing too.
Here are some of its key features that matter most:
Touch-sensitive gain adjustment: fingertip precision helps when you’re scanning fast or in low-light exam rooms.
Advanced imaging tools: HR Flow for detailed blood-flow visualization, iClear speckle noise reduction, one-click image optimization (iTouch), natural-touch elastography, contrast imaging.
Vet-specific workflow features: Smart Calc (automatic lesion tracing/measurement), Smart HRI (quantitative liver steatosis assessment), iWorks animal-specific scanning protocols, and iReport customizable professional report templates.
Portable and adaptable: Lightweight for mobility (if you offer mobile service, or move between treatment rooms), multiple connectivity options, quick probe switching, and ample storage capacity.
All of these features make this a standout option when you’re seeking more than just “basic” without stepping into ultra-premium cost territory.
ROI: How to Make the Numbers Work
Let’s look at a hypothetical ROI scenario for a hospital adding the Vetus E5.
Assumptions:
You perform four extra ultrasound scans per week that you couldn’t before (let’s say conservatively).
Charge $250 per scan (typical value will vary by region and case type).
That’s $1,000 in additional weekly revenue → roughly $52,000 per year.
Even if you account for consumables, training time, and service/support costs, you could recoup the investment within the first year and then benefit from what follows.
Other benefits to consider:
Fewer referrals out, meaning more revenue stays within your hospital.
Enhanced client confidence, resulting in more return visits and more word-of-mouth.
Faster diagnostics = better outcomes = higher throughput.
Marketing value, meaning you can promote “in-house advanced ultrasound” and attract clients who previously went elsewhere.
In other words, for a one-time investment, you can unlock significantly more diagnostic capacity and revenue potential.
How to Decide if It’s Right for Your Hospital
Here are a few questions to think about:
What’s your patient mix and demand? Do you have a volume of cases where soft-tissue imaging, cardiac screening, and abdominal ultrasound are becoming more frequent?
What are your current limitations? Are you referring out because you don’t have an in-house unit? Are you missing revenue because you can’t scan quickly or confidently?
Probe and accessory plan: What probes will you need right away (convex, linear, phased array)? What future add-ons might you want?
Service/support and total cost of ownership: What support is provided? What warranty, what response time? What consumables or service contracts will you need?
Integration into your hospital’s workflow: Can the system connect to your practice management/PACS system? Are image-sharing/reporting features compatible?
If you answer these honestly and the Vetus E5 meets the criteria, you’re making a firm decision.
Practical Tips for Implementing Your New Ultrasound
Plan a “go live” day: Set aside time for staff training and run sample scans before full use. Make sure your team feels comfortable using the new tool before you’re in full swing.
Create scanning protocols: Standardize for common cases (e.g., feline abdominal, canine cardiac, reproductive scans) to make your team more efficient, consistent, and confident.
Advertise your new capability: Use your website, newsletters, and social media to let clients know you now offer comprehensive in-house ultrasound.
Monitor usage: After implementation, track the number of scans per week, average revenue per scan, and the reduction in referrals. Use these metrics to evaluate success.
Schedule maintenance and service reviews: Keep the system at peak performance and avoid downtime that could delay cases or cause referral leakage.
Expand Your Service Capacity
Upgrading diagnostic capabilities doesn’t have to mean spending top dollar. With the Vetus E5, your hospital can invest in a robust, veterinary-specific ultrasound system and dramatically expand your service capacity. You gain advanced imaging tools and workflow efficiency—and a clear path to ROI.
The right imaging tool doesn’t just make your life easier—it elevates your practice. It allows you to say “yes” more often to cases, it keeps clients in-house, and it helps your team deliver better patient care.
Proving ROI: Making the Case for In-House Veterinary Imaging
Investing in new imaging equipment, whether it's a digital X-ray system, dental X-ray, or ultrasound, can feel like a big leap. The price tag is upfront and very real… but so is the return when the equipment is used effectively.
The challenge can be convincing everyone else on your team of their value.
The good news: in-house imaging is one of the easiest investments to justify when you know which metrics to measure.
Let’s break down the key numbers that actually matter and how to present them so your team understands and supports them.
1. Start With Imaging Volume
Most practices use imaging more often than they realize.
But because they’re outsourcing cases or relying on outdated equipment, they underestimate the number of opportunities available to them.
What to measure:
How many X-rays or ultrasounds do you currently perform each month
How many do you refer out
How many cases do you skip altogether because of logistics, client cost, or scheduling limitations
A practical example:
Let’s say a 3-doctor practice:
Takes ~70 in-house X-rays/month
Refers out 20+ imaging cases/month
Has an estimated 10–15 “missed opportunities” where imaging would have helped, but wasn’t pursued
That’s 100+ cases per month that a modern digital X-ray system or ultrasound system could capture.
If your average imaging fee is $150–$250, that’s:
$15,000–$25,000 per month in potential revenue.
Even if you estimate conservatively, you can quickly show that the equipment pays for itself—often in less than a year.
2. Case Conversion Rate: The Metric Nobody Talks About
You’ve probably seen this… when imaging is easy, fast, and available right now, more clients say “yes.”
When imaging requires a referral, a second trip, or more money upfront… fewer clients say yes.
What to measure:
Percent of recommended imaging that clients accept today
The percent you expect once imaging is same-day and in-house
Some practices that started offering same-day digital X-rays increased their acceptance rate from 43% to 78% in the first 3 months.
Why? When imaging is immediate, convenient, and clearly explained, clients see the value.
This means:
More complete diagnostics
More accurate treatment plans
More revenue per visit
Better medical outcomes—your team will care about this point as much as the financials.
Increasing your case conversion rate by even 15–20% can add thousands in monthly revenue without adding any new clients.
3. Referral Retention
Referrals aren’t bad by any means; you often need specialists.
But referring out basic imaging is one of the biggest hidden drains on revenue.
What to measure:
How many imaging referrals do you send out monthly
Average cost clients pay externally
Percent of referred clients who don’t return for follow-up care
Missed procedure revenue because the patient went to another hospital
If you refer out 20–30 ultrasounds per month at ~$300 each, that’s $6,000–$9,000 monthly handed to another practice.
Keeping even half those cases in-house often justifies the cost of a mid-range ultrasound system or DR panel on its own.
4. Cost Avoidance
Sometimes, it’s not about the revenue you gain but the expenses you stop paying.
What to measure:
Outsourcing fees (radiographs, dental films, ultrasounds)
Additional sedation or handling charges caused by slow equipment
Time cost from workflow delays
The cost of retakes with outdated systems
A practice relying on outdated or low-resolution ultrasound equipment might:
Spend 15–20 extra minutes per scan due to slow boot-up times, poor image acquisition, or difficult navigation
Require additional restraint or sedation for anxious or painful patients because older probes take longer to capture clear images
Delay treatment decisions while waiting for images to be reviewed, re-taken, or sent out for interpretation
Upgrading to an ultrasound system can save:
10+ hours/month of staff time through faster image acquisition and streamlined workflows
5–10 sedation or heavy restraint events by reducing scan times and improving patient comfort
Countless repeat scans and workflow disruptions, thanks to enhanced image quality and intuitive controls
That’s real money saved, even before you consider the revenue side.
Putting It All Together
Most veterinary practices already have the patient volume to justify in-house imaging; they haven’t measured it yet. When you break down the numbers, the ROI becomes obvious:
More case conversions
Higher client satisfaction
Better patient outcomes
Faster workflows and a rapidly recouped investment
If you’re preparing to make the case to your team, this framework gives you everything you need to build confidence and get buy-in.
A Veterinary Ultrasound Buyer’s Guide
Choosing the Right Veterinary Ultrasound
For veterinary practices, investing in the right ultrasound system is more than just buying a machine — it’s about choosing a tool that fits your patients, workflow, and long-term goals.
Below is your guide to making smart, confident decisions when selecting the best ultrasound for your hospital.
1. Key Factors When Purchasing a Veterinary Ultrasound
Imaging Performance and Probes
The types of patients you serve — small animals, equine, or exotics — will determine your probe requirements. Look for technologies such as Doppler flow imaging, speckle reduction, and image clarity enhancements, and make sure probe switching is simple and efficient.
Workflow Integration and Veterinary-Specific Features
Ease of use is crucial, especially in a busy practice. Look for intuitive controls, veterinary presets, reporting tools, and connectivity to PACS or practice management software. If your practice includes mobile or fieldwork, portability should be a top priority.
Service, Warranty, and Support
The best technology is only as strong as the support behind it. Check for service plan options, local support, parts availability, and software upgrade pathways to ensure long-term reliability.
Investment and ROI
The initial investment is just the beginning. Include maintenance, training, probes, and consumables when evaluating overall value. Estimate how many scans you’ll perform weekly or monthly, and your revenue per scan, to calculate your break-even point and expected ROI.
2. Value-Focused Option for Small or General Animal Practices
For practices seeking high capability and a balanced investment, the Mindray Vetus E5 is an excellent choice.
Key Features
- Touch-sensitive gain adjustment for fingertip precision
- Intuitive control panel designed for veterinary use
- Advanced imaging: one-click optimization (iTouch), speckle-reduction (iClear), HR Flow, natural-touch elastography, and contrast imaging
- Lightweight and portable for in-clinic or mobile use
Why It Matters
This system offers strong value and a fast ROI. Its versatility across small and mixed animal applications — abdominal, soft tissue, cardiac, and reproductive — makes it a solid all-around investment for general practices.
3. Specialized Option for Equine and Large-Animal Practices
For equine or mixed-animal veterinarians, the Mindray Vetus EQ is a purpose-built system that delivers premium performance and portability.
Key Features
- Includes two transducers from options such as C5-1s convex, L13-3Ns linear, P4-2s phased array, or 6LE5Vs probes
- Extremely portable: weighs only 6.5 lbs and just 1.73″ thick
- 15.6″ LED monitor plus 12.3″ anti-glare touchscreen for barn or field use
- Preloaded equine presets: musculoskeletal, cardiac, abdomen, and reproduction
- Powered by ZST+ Zone Imaging technology for excellent image clarity and penetration
Why It Matters
Large animals require deeper imaging, a wider field of view, and durable equipment that performs well in challenging environments. The Vetus EQ is designed for these conditions — offering the portability, clarity, and ruggedness needed for on-farm or mobile work.
4. Key Questions to Ask Your Equipment Distributor
- What is included in the base package (probes, software, warranty)?
- What upgrade options are available (additional probes, software modules, reporting tools)?
- What service and support plans are offered (onsite vs. remote, response time, preventive maintenance)?
- How is training handled for your team?
- What are the consumable costs, warranty terms, and what happens if a probe fails?
- How compatible is the system with your current digital workflow (DICOM, PACS, practice management software)?
- What ROI timeline can you expect based on your case volume and patient mix?
5. Smart Decisions Made Easy
Ultrasound remains one of the most versatile and profitable diagnostic tools in veterinary medicine. Choosing the right system helps you improve patient care, expand diagnostic capabilities, and grow revenue.
Partner with a trusted distributor who provides not only the hardware, but also training, support, and integration guidance. That’s how your new ultrasound becomes more than just another machine — it becomes a vital tool for better diagnostics and sustainable practice growth.
8 Workflow Mistakes Undermining Your Diagnostic Equipment Investment
Diagnostic Imaging for Veterinary Practices
Explore our most requested systems, then review the workflow playbook below to maximize your ROI.
Avoid These 8 Imaging Workflow Errors in Vet Clinics
Investing in new diagnostic equipment, whether it’s a digital X-ray, ultrasound, or in-house lab analyzers, is one of the most impactful decisions a veterinary practice can make. But even the best technology can fall short if efficient workflows don’t support it.
It’s not uncommon for practices to purchase cutting-edge equipment only to find it underutilized, creating bottlenecks or staff frustration. The good news? These issues usually come down to workflow—not the equipment itself.
Here are eight common workflow mistakes that can quietly undermine your investment—and how to fix them.
-
Inadequate Staff Training
One brief demo at installation isn’t enough. Inconsistent or incomplete training leads to errors, slowdowns, and missed diagnostic opportunities.
The fix: Schedule comprehensive hands-on training for all relevant staff and create clear SOPs for each device. Assign a “champion user” to support ongoing training, maintenance, and onboarding.
-
Poor Equipment Placement and Room Layout
Cramped or inconvenient placement disrupts flow—staff travel farther, cross paths, and squeeze around tables, increasing time per case.
The fix: Map the workflow before installation. Place frequently used equipment near treatment/exam areas and ensure proper clearance for patients and staff.
-
Not Integrating With Your Practice Software
Without PIMS integration, teams waste time on manual data entry and risk transcription errors.
The fix: Work with your provider to ensure full integration. Enable direct image uploads and automatic results imports to save time and improve accuracy.
-
Overlooking Preventive Maintenance
Skipping maintenance or calibration causes inconsistent image quality and unexpected downtime.
The fix: Treat maintenance like patient appointments. Use a service plan for inspections, cleanings, and calibrations on schedule.
-
Not Adjusting Scheduling and Staff Roles
New technology changes patient flow. If schedules and roles don’t adapt, you’ll see idle time or backlogs.
The fix: Reassess after installation. Consider dedicated techs for diagnostics during peak times, or add “diagnostic blocks” to your calendar.
-
Ignoring Change Management
Team resistance can mean inconsistent use or reluctance to adopt new processes.
The fix: Involve the team early. Share the “why,” invite feedback, and celebrate quick wins to build buy-in.
-
Underutilizing the Equipment’s Full Capabilities
Advanced features—contrast tools, cloud storage, automated reporting—often go unused.
The fix: Schedule periodic check-ins with your distributor or manufacturer. Ask about updates, features, and best practices to unlock more value.
-
Failing to Measure Performance
If you don’t measure usage and outcomes, you can’t prove ROI or improve bottlenecks.
The fix: Track studies per month, time from imaging to diagnosis, and referral cost reductions. Use insights to refine workflows and highlight clinical/financial impact.
Supportive Workflow Makes a Difference
A successful diagnostic upgrade isn’t just about the technology—it’s about the workflow that supports it. With thoughtful planning, proper training, and regular review, your new equipment can enhance efficiency, patient care, and profitability for years to come.
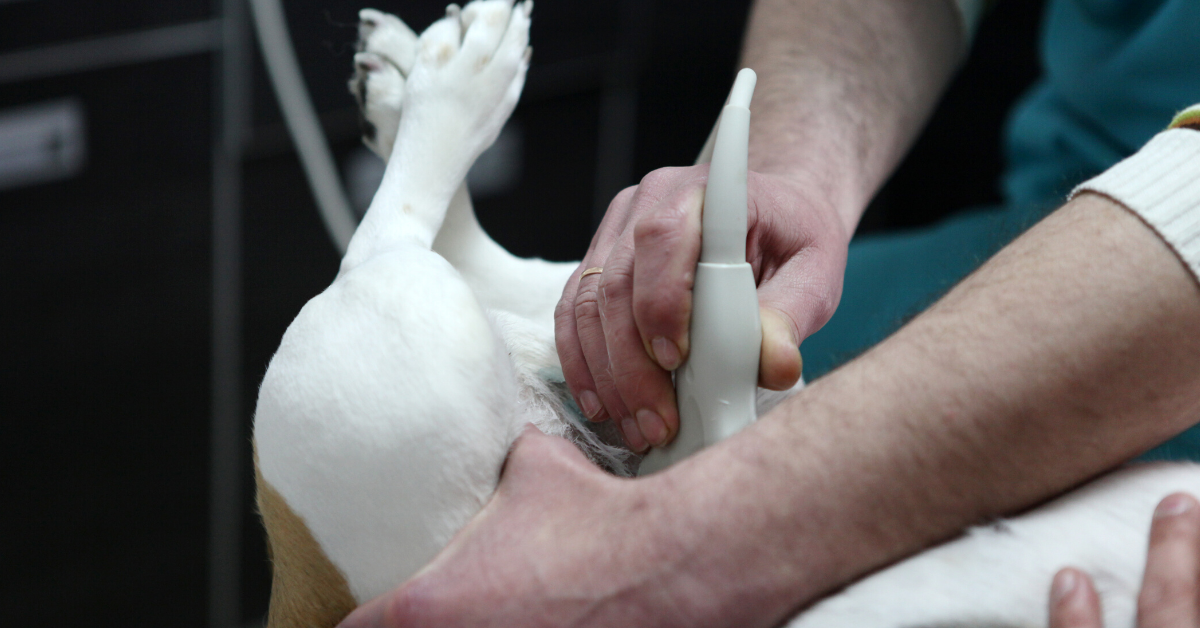
Why Your Vet Clinic Needs Ultrasound for Safer Cystocentesis
Ultrasound Makes Cystocentesis Less Stressful for All
In veterinary medicine, minor improvements in technique can make a big difference.
One of those game-changing tools is ultrasound, particularly when it comes to performing safer, more reliable cystocentesis.
Suppose your practice doesn’t already use ultrasound for this everyday procedure. In that case, you may be missing an opportunity to improve diagnostic quality, reduce stress (for everyone involved), and elevate the standard of care you offer.
Here’s why it’s worth investing in — and how it can transform how you approach even routine diagnostics.
Cystocentesis Without Guesswork
If you’ve ever performed a blind cystocentesis on an obese dog, a wiggly cat, or a patient with a tiny, poorly palpable bladder, you know how tricky it can get.
Even with years of experience and skilled hands, there’s a level of uncertainty — are you truly in the bladder? Is it full enough? Are you avoiding other organs?
Ultrasound eliminates the guesswork
With real-time imaging, you can see exactly where the bladder is and guide your needle precisely, even when the bladder is small, displaced, or hidden by fat or intestines.
This not only improves your confidence but also makes the procedure faster and less stressful for the patient.
Let’s look at an example…
Take Blaze, for instance—a senior cat with chronic kidney disease who presents for a urine culture. On palpation, her bladder feels small and challenging to locate. With ultrasound, you can quickly find the small dorsal bladder and collect a sample without repeated attempts — a win for you, your patient, and the client.
Why Safer Matters — Beyond the Obvious
Of course, accuracy is essential, but safety is equally critical. Blind cystocentesis carries risks that can be mitigated with ultrasound:
Puncturing the intestines or uterus by mistake
Traumatizing bladder tumors or inflamed tissue
Causing unnecessary discomfort with multiple unsuccessful attempts
With ultrasound, you can avoid these pitfalls by choosing the safest access point and observing the bladder’s walls and contents before you proceed.
It also builds trust with clients. Being able to explain, “We used ultrasound to guide our sample collection and avoid complications,” reassures pet owners that you’re providing the best care possible.
Unexpected Perks for Your Practice
Adding ultrasound for cystocentesis also brings less obvious benefits:
Team empowerment: Veterinary technicians can be trained to perform ultrasound-guided cystocentesis under supervision, freeing doctors for more complex tasks.
Time savings: Fewer failed attempts mean shorter appointments and happier patients.
Professional pride: Offering a more advanced and refined approach sets your clinic apart, signaling to clients that you prioritize precision and patient comfort.
Overcoming Barriers to Getting Started
You might wonder: Isn’t ultrasound overkill for something as simple as cystocentesis?
Not anymore.
Modern ultrasound units are more affordable, portable, and user-friendly than ever — and they’re designed with veterinary needs in mind.
Training doesn’t have to be a hurdle, either. Many manufacturers offer resources to help you and your team get comfortable with the technology quickly.
And once you’re familiar with it, you’ll find yourself reaching for ultrasound not just for cystocentesis but for countless other applications — from pregnancy checks to identifying abdominal masses.
Ready to Upgrade Your Standard of Care?
By incorporating ultrasound into cystocentesis, your team can make this routine procedure safer, more precise, and less stressful for everyone involved.
From improving sample quality to reducing complications, ultrasound guidance offers clear benefits that elevate patient care and strengthen client trust.
It’s a simple-but-powerful way to advance the quality of medicine you provide every day.
Explore the ultrasound systems we offer:
Mastering Cystocentesis: Benefits of Ultrasound Guidance in Veterinary Medicine
Top Benefits of Ultrasound-Guided Cystocentesis
Cystocentesis is a cornerstone diagnostic procedure in veterinary medicine; however, even for experienced teams, it can present its challenges.
Fortunately, ultrasound guidance has revolutionized how we perform this critical task, making it safer, more accurate, and more efficient.
Let’s take a moment to explore the benefits of ultrasound-guided cystocentesis and discuss common challenges — as well as how to overcome them — so your team can master this procedure with confidence.
Why Upgrade to an Ultrasound-Guided Cystocentesis Method?
Traditionally, cystocentesis was done “blind,” using only palpation to locate the bladder. While this can work well in ideal patients — those who are lean, cooperative, and have a full bladder — not all patients fit that description.
Ultrasound-guided cystocentesis gives you:
Precision: Visualize the bladder in real time and guide your needle directly into it, reducing the risk of accidental injury.
Cleaner samples: Essential for urine cultures, especially when diagnosing infections or bladder disease.
Improved safety: Paramount in patients with small bladders, obesity, or abdominal masses, where blind cystocentesis risks puncturing other organs.
Confidence under challenging cases: For example, in a tense cat with hematuria, ultrasound helps you find and access even a small, hard-to-palpate bladder.
Let’s say Johnny, a middle-aged male cat, presents with straining and blood in his urine. On palpation, his bladder feels small and difficult to isolate. With ultrasound, you can see the partially contracted bladder nestled beneath intestinal loops, allowing you to confidently and safely obtain a diagnostic sample on the first attempt.
Tips and Best Practices for Success
Choose the proper probe:
A microconvex or linear transducer is ideal for small animal abdominal imaging because it offers good resolution and fits easily against the body wall.
Positioning matters:
Most patients do well in dorsal or lateral recumbency. Ensure the patient is calm — sometimes gentle sedation or a quiet room can make all the difference.
Scan before you poke:
Before inserting the needle, take a moment to thoroughly scan the bladder. Identify its borders, note any stones, masses, or unusual anatomy, and plan your needle path.
Use the in-plane approach:
Whenever possible, guide your needle within the ultrasound beam so you can watch its entire length — and the tip — enter the bladder.
Have an assistant help:
A trained veterinary technician can hold the probe steady while you guide the needle, keeping your hands free and maintaining a clear image.
Common Challenges and How to Overcome Them
Even with Ultrasound, you may encounter some hurdles. Let’s talk it through…
The bladder is too small: Some patients present after voiding or have a chronically small bladder (e.g., due to polyuria).
Solution: If the sample isn’t urgent, wait and give the patient access to water. You can also use a fluid bolus and monitor until the bladder refills enough to access safely.Obese or tense patients: In these patients, the bladder can be obscured by fat or muscle tension.
Solution: Position them carefully to minimize pressure on the abdomen and consider mild sedation to relax abdominal muscles.Needle not visible: If you can’t see the needle on the ultrasound screen, it’s likely off-plane.
Solution: Adjust your angle and make small movements while watching the screen until the needle comes into viewPatient movement: Sudden movements can make it hard to keep the bladder in view and the needle steady.
Solution: Enlist a skilled technician to hold the patient securely and calmly. In some cases, light sedation may be appropriate.
A Team Effort — And a Growth Opportunity
Ultrasound-guided cystocentesis isn’t just a skill for veterinarians — it’s also an excellent way for veterinary technicians to grow professionally. With appropriate training, technicians can perform this procedure competently, freeing up doctors for more complex tasks and improving overall hospital efficiency.
Invest in the Right Tools
Of course, mastering ultrasound-guided cystocentesis starts with the right equipment. High-quality imaging, ergonomic probes, and user-friendly interfaces make it easy for your team to perform accurate, confident diagnostics every day.
With the right equipment, a little practice, and teamwork, this procedure can become second nature — and a true diagnostic advantage!
Links to the systems we offer:
https://newvetequipment.com/vetus-e7-ultrasound
https://newvetequipment.com/vetus-9-veterinary-ultrasound-system
https://newvetequipment.com/vetus-eq-ultrasound-system
https://newvetequipment.com/basic-bladder-scanner-by-mindray
Ultrasound-Guided Cystocentesis: Precision for Veterinary Diagnostics
Why Ultrasound Is Now Standard for Cystocentesis
In our line of work, accuracy is one of the most crucial factors in ensuring a clean sample collection and an accurate diagnosis. When it comes to diagnostic procedures like cystocentesis, precision has a direct impact on patient outcomes, sample quality, and client satisfaction. That’s why ultrasound-guided cystocentesis is becoming the gold standard in veterinary practices everywhere.
Whether you're a seasoned practitioner or building a new hospital, integrating ultrasound guidance into routine procedures like cystocentesis can enhance the quality of care and improve diagnostic reliability.
It’s a win-win! But, before we get ahead of ourselves, let’s break it down…
What is Ultrasound-Guided Cystocentesis?
Cystocentesis is the percutaneous aspiration of urine from the bladder using a needle and syringe.
Traditionally, it’s performed by palpating (or feeling) the bladder manually, which can be effective in some cases, but not all.
Ultrasound-guided cystocentesis takes this a step further by using real-time imaging to guide the needle directly into the bladder, offering unmatched precision and reducing guesswork.
Why Use Ultrasound Guidance?
1. Increased Accuracy
One of the main advantages of ultrasound guidance is visual confirmation of bladder location, size, and wall integrity. This is especially helpful in:
Obese patients where palpation is difficult
Nervous or tense animals that guard their abdomen
Patients with small or partially voided bladders
Critical care patients who cannot be positioned ideally
By directly visualizing the bladder, we can ensure correct needle placement and avoid surrounding structures such as the intestines or uterus, significantly reducing the risk of complications.
2. Improved Sample Quality
When you’re aiming for a sterile urine sample for culture or cytology, contamination is a concern.
Palpation-based cystocentesis increases the risk of dry taps or puncturing non-target tissues, which can compromise the quality of the sample.
Ultrasound guidance minimizes these risks, resulting in cleaner samples, a higher diagnostic yield, and greater confidence in the results. This is particularly valuable when investigating things like:
Urinary tract infections
Hematuria
Bladder masses
3. Greater Safety for Challenging Cases
In some instances, like patients with transitional cell carcinoma (TCC), cystoliths, or anatomical abnormalities, can be more safely evaluated with ultrasound guidance. You can:
Avoid needle contact with neoplasms
Visualize and avoid stones
Confirm bladder fullness before attempting the procedure
This reduces the chance of iatrogenic injury (injuries caused by the needle) and aligns with best practices for minimally invasive care.
Now that we’ve got the basics covered, let’s unpack what good looks like for this particular procedure.
Tips and Best Practices for Ultrasound-Guided Cystocentesis
1. Use the Right Equipment
Invest in an ultrasound machine with high-resolution imaging and a microconvex or linear transducer; both are ideal for abdominal imaging in small animals. Having a veterinary-specific machine ensures preset parameters are optimized for soft tissue visualization.
Pro Tip: Use a hands-free probe holder or enlist a trained assistant to hold the transducer while you guide the needle. This helps maintain image stability and needle visibility.
2. Positioning Matters
Dorsal or lateral recumbency usually works best. Use gentle restraint to reduce stress and abdominal guarding. A calm, cooperative patient makes the procedure easier and more comfortable for everyone.
3. Visualize the Entire Path
Before inserting the needle, scan the full path from the skin surface to the bladder. This helps you identify any vessels, intestines, or abnormalities that could interfere with the procedure.
4. Use the In-Plane Technique (When Possible)
The “in-plane” approach is an ultrasound-guided technique in which the needle is inserted along the same plane as the ultrasound beam, allowing the entire length of the needle (including the tip) to be visible on the screen as it advances toward the target (in this case, the bladder).
Let’s look at it in action…
A 9-year-old spayed female Labrador retriever, Mila, presents with hematuria and pollakiuria, resulting in blood in her urine and frequent urges to urinate. On abdominal palpation, the bladder feels small and difficult to isolate. Rather than risk multiple blind attempts, her veterinarian uses ultrasound guidance. The bladder is visualized dorsal to the pubis, partially obscured by intestinal loops.
With the ultrasound probe held steady, a 22-gauge needle is guided in-plane, avoiding bowel loops and penetrating the bladder wall cleanly. A 7 mL urine sample is collected with no complication, and the diagnostic yield from both urinalysis and culture is high.
The client receives fast, accurate results, and the patient avoids the stress of repeat attempts or complications.
Is Your Practice Equipped for Precision?
Integrating ultrasound-guided techniques like this one isn’t just about upgrading your technology; it’s about upgrading your standard of care.
Not to mention, this is an excellent opportunity for veterinary technicians to enhance their clinical skill set while improving workflow efficiency within the practice.
With proper training, technicians can confidently perform this procedure, ensuring accurate sample collection and patient comfort.
By taking on this advanced task, technicians help free up the veterinarian’s time for more complex diagnostics, treatments, or client communication—ultimately enhancing the hospital’s overall productivity and quality of care.
Ultrasound-guided cystocentesis brings precision, safety, and diagnostic confidence to a routine veterinary procedure. As pet owners increasingly expect modern and accurate diagnostics, ultrasound is becoming the gold standard.
Links to the systems we offer:
https://newvetequipment.com/vetus-e7-ultrasound
https://newvetequipment.com/vetus-9-veterinary-ultrasound-system
https://newvetequipment.com/vetus-eq-ultrasound-system
https://newvetequipment.com/basic-bladder-scanner-by-mindray
10 Steps To Complete Dental Cleaning Procedures In Pets
Perform a pre-anesthetic checklist, including patient history, exam, lab work, chest X-rays, and prophylactic medications, especially for senior patients.
Ensure all equipment is functioning properly and that all essential instruments are available and sanitized. Ensure the CPR plan and CPR medications are in place, as well as resuscitation status for each patient.
Provide a safe heat source such as a warm air blanket.
Continually check the patient by placing your hand directly on the patient under the heat source. Include this step on your anesthesia monitoring sheet.
Ensure the patient is warm during the pre-anesthetic phase where a patient’s body temperature can lower.
1. During the onset of anesthesia while intubating, use caution when handling the tongue, ensuring it is not pulled forcefully. Gently place the patient in position – note; placing a pet on their back during the entire procedure minimizes anesthesia time and is an effective and expeditious way to perform a dental.
Ensure the tracheal tube is adequately inflated, and an aspiration guard or gauze is in place. Consider the use of intraoral suction to prevent aspiration of water and debris during the procedure.
Continually replace gauze as it becomes saturated with water. Continually check the tracheal tube during the procedure as it may need adjusting depending on the depth of anesthesia and tracheal relaxation
2. While under anesthesia, take before and after photographs of all areas of the mouth to show the pet parent, as well as keep for documentation in the medical record.
3. Begin by irrigating the pet’s mouth with a dilute Veterinary Oral Health Council approved Chlorhexidine based rinse such as CET. Evaluate the oral cavity, and remove obvious calculus at this time to expose gingiva and soft tissues.
4. Perform intraoral regional nerve blocks prior to probing the teeth and gingival tissues, as this procedure may cause pain in the anesthetized patient, requiring a deeper plane of anesthesia.
5. Thoroughly probe and chart each tooth, and perform full-mouth radiographs
6. Clean the teeth, perform extractions, and required orthodontic procedures needed. Ensure hand scalers and a curette are employed to remove subgingival calculus, particularly where periodontal pockets have been identified.
7. Thoroughly irrigate and lavage away oral debris.
8. Polish all surfaces of each tooth and subgingival areas thoroughly and carefully.
9. Rinse the mouth and each tooth with air and water and ensure all debris is removed from the tongue. Take post-procedure photographs.
10. Finally, apply a plaque prevention gel or dental sealant
Recover the patient quietly and employ pain management and anti-inflammatory medication. The post-anesthetic patient should be monitored closely post-surgically.
Written by: Dr. Tammy Powell, DVM
Ultrasound Tips: Evaluating GI Tract Issues in Cats and Dogs
An abdominal ultrasound is a tool that can help you with visualizing and diagnosing a variety of conditions in your canine and feline patients.
Today, we’ll be talking about evaluating the gastrointestinal tract.
Depending on your patient, you may be doing an ultrasound exam of the stomach, small intestines, and colon to look for…
Inflammation and wall thickening
Foreign bodies
Neoplasia
Pyloric outflow obstructions
Intussusceptions
Enlarged mesenteric lymph nodes
This isn’t an exhaustive list…
But basically, if the patient is having GI symptoms and your x-rays haven’t provided the answer you need, an ultrasound is often a good next step.
That’s because it provides more details about tissue structure in real-time, as opposed to just the silhouette of radiographs. Often, x-rays and ultrasound work well together.
It may take a little bit of practice, but with experience you can catch on to ultrasound technique and do your ultrasound exams in-house rather than referring.
Here are a few tips for getting the diagnostic information you need during a simple ultrasound evaluation of the GI tract…
If possible, have the patient fast beforehand. That way, you can get a clear picture of the GI tract without a lot of food or fecal matter to block your view of certain structures or create artefacts such as shadowing. You can also consider an enema if needed.
Position the patient. Dorsal recumbency is most common, although lateral recumbency may also be used, especially for visualization of deeper structures. Use a trough for comfort, and if appropriate consider sedation (most patients don’t need to be sedated, though).
Experts recommend having a systematic approach to look at the entire abdomen. Whichever viewing order works best for you, it’s good to be consistent so nothing is forgotten. And, the GI tract will be an important part of your evaluation.
Choose a machine and probe that work best for your needs, then practice and develop comfort using the different settings, especially adjusting depth and gain (brightness). That way, you can focus on seeing what you want to see, rather than fussing with settings during your ultrasound exam.
Start at the stomach by locating it just caudally to the liver. Rock and fan the probe to systematically obtain orthogonal views of the whole stomach from fundus to pylorus.
Next, examine the intestines and cecum.
The duodenum, ileum, cecum, and colon are examined individually.
For the jejunum, you don’t need to follow every loop from beginning to end. Instead, scan the abdomen starting at the level of the stomach. Slide or sweep the probe from side to side, gradually moving cranially to caudally until you’ve visualized the entire field (usually you would stop at the level of the urinary bladder trigone).
Along the way, take notes to help you prepare your report for your patient’s medical record. Be sure to include what was normal, as well as any abnormalities you found, such as masses or thickened intestinal walls.
While scanning, you can freeze images for your records and take measurements if you feel anything may be enlarged.
When you develop your ultrasound skills, having this tool at your disposal can often give you quick information when you need it—for example, looking for a GI mass or obstruction when x-rays were inconclusive.
It’s a great way to offer an additional service to your patients and clients, and possibly to stand out from other clinics in your region.
Written by: Dr. Tammy Powell, DVM
Patient Injury & Complications In Veterinary Dentistry
The nature of anesthesia brings risk in general. In veterinary medicine, during dental procedures, pets are often placed in vulnerable positions which can lead to increased risk of injury and medical complications.
These risks can be minimized or entirely avoided with careful consideration, and proper training and continuing education of staff. Listed are a few of the more common injuries that can occur during a dental procedure.
Aspiration Pneumonia
Aspiration pneumonia in pet patients occurs when the patient inhales a foreign substance and develops lung inflammation and infection as a result.
The most common occurrence during dentistry is water and debris entering an unprotected airway, hence allowing fluid and debris to enter the lungs. This can occur from an underinflated tracheal tube, or repositioning during the procedure that allows fluid to enter the airway.
Aspiration pneumonia can also occur if the patient vomits or regurgitates during anesthetic recovery.. To reduce the incidence of dental-related aspiration pneumonia, maintaining the patient on their back during the procedure, and avoiding repositioning has proven to not only lessen the risk of aspiration but also lessens the amount of anesthesia needed during the procedure.
In addition, antiemetic medications given during the premedication phase can help reduce the incidence of post-anesthetic nausea and vomiting. Caution should be taken during the recovery phase to wait until the patient is alert and responsive enough to deflate the cuff and remove the tracheal tube.
Tracheal rupture
Tracheal rupture in dogs and cats are more frequent during dental procedures than any other medical procedure. Seventy-five percent of tracheal ruptures are thought to be associated with oral surgical procedures with the incidence more common in cats than dogs.
Tracheal injury can cause symptoms such as mild dyspnea, and even death. The most likely cause of tracheal rupture is thought to be due to an overinflated tracheal cuff, as well as failing to detach the tracheal tube from the anesthesia hose during repositioning, which can cause a torque on the inflated cuff resulting in a tear of the dorsal membrane of the trachea.
Another common cause of tracheal rupture is a patient that is not adequately anesthetized and coughs or lunges upward during intubation, tearing the trachea.
Pressure from an overinflated cuff can cause pressure necrosis of the trachea, showing delayed symptoms of inflammation and scarring.
Avoiding over-inflation of the cuff, using new tracheal tubes, testing the cuff to ensure proper inflation prior to use, avoiding repositioning as much as possible, and ensuring a level plane of anesthesia prior to intubation can help minimize the risk of tracheal rupture.
Artery Damage during Tooth Extractions
Arterial damage to arteries such as the palatine artery which runs the length of the mandible can accidentally occur during routine tooth extractions where the instrument can slip from the practitioner’s hand.
These injuries can be mild to more severe requiring surgical intervention.
The most effective way to avoid this type of injury is to implement extraction techniques involving gingival flaps where the roots are exposed, and more easily undermined, and extracted.
Written by: Dr. Tammy Powell, DVM
Sell Your Used Veterinary Equipment On A Community Website
Sell Your Used Veterinary Equipment
Welcome to the other half of our series on buying and selling your used equipment on usedvetequipment.com.
If you’re looking to sell some of your equipment, you’re not alone. There are many reasons why you might pursue this option as a veterinarian…
Maybe that new in-house chemistry analyzer or the extra kennels you purchased didn’t get used as much as you expected—and you’re not seeing the return on investment you wanted…
Maybe you want to upgrade, but you aren’t sure what to do with your current equipment. Or, maybe times are tight and you need to increase your cashflow.
Whatever your reason, selling your used veterinary equipment can put some cash in your pocket, while also helping out a fellow member of the veterinary community who needs the machine, gadget, or gear you’re selling.
If that sounds great to you and you’re ready to get started, we recommend visiting usedvetequipment.com. Here’s why…
List Anything! Whether you’re looking to sell an ophthalmoscope, an autoclave, an x-ray processor, or a vehicle… there’s no item too large or too small.
Set Your Own Price. You choose how much you’d like to sell for, and you can accept or reject any offer that comes your way.
We’re Here to Help. We’ve done this thousand of times—so no matter what you need to ship, we can help you with logistics and also ensure prompt payment from your buyer.
Since this is a community-based platform, you’ll find interactions to be secure, reliable, and honest.
Affordable. There’s no cost to you to list your equipment (including unlimited photos and videos to showcase your items), and no time limit in which to sell.
Good for Animals and the Environment. Reusing and repurposing equipment is not only a great way for the veterinary community to share resources to improve animal care everywhere—but it can also help keep materials out of landfills.
Stellar Service. Just check the site, and you’ll find reviews from tons of happy buyers and sellers! Like this one below…
“I can’t say enough about the great job Brad did in selling our cages and floor grates. It was quick and everyone is happy. Brad found the right buyers and made all the arrangements. I highly recommend this website.”
—JS in NY
Selling is simple on usedvetequipment.com. But, we also have some tips to help you get the most success out of your listing.
For the most success when you sell your equipment, be sure to include…
Pictures! You can include as many pictures as you’d like to on your listing, and video if that will help to show your item.
Images will help your equipment sell—and most smartphones are perfectly capable of producing the high-quality photos you need.
Try photographing from different angles, cleaning the items before you take pictures, and removing any distracting clutter from your shot so the focus is solely on the equipment you’re selling.
Detailed Descriptions. Include all relevant details about the brand name, manufacture date, current condition, size and weight, the reason for selling, etc.
Also, let potential buyers know how the item has helped you in your daily practice—and how it can help them.
A Smart Pricing Strategy. Sometimes, pricing used equipment appropriately can be difficult—you know there will be some depreciation, but what’s a fair price?
The easiest way to get a starting point is to research similar items that have recently sold.
And, if you’re hoping to sell fast—it helps to go a little under the going rate or to include shipping in your price.
And that’s it! Once your equipment is listed on usedvetequipment.com, you can easily connect with colleagues who are interested in buying.
With each sale, that’s money you can invest back into your practice for expanding, upgrading, marketing, or compensating your amazing team members.
Plus, you’d be helping out a fellow practitioner in the veterinary community—someone who really wants the equipment you don’t need anymore. It’s a win-win for both of you.
Good luck, and happy selling!
“I had an entire Veterinary Clinic of items to sell and Brad sold them all! He is diligent in getting items sold and payment is speedy. Brad and UsedVetEquipment.com are The Best!”
—S.F. in Colorado
“Brad was able to sell my cages within a week of posting the items. He had great communication and payment was prompt. I will list my items with him again.”
—Wes Godwin - Texas
Written by: Dr. Tammy Powell, DVM
Mastering Ultrasound-Guided Cystocentesis in Dogs and Cats
There are several ways to collect a urine sample from your patient, including free catching, using a urinary catheter, and doing a cystocentesis.
A cystocentesis—which involves obtaining a urine sample via a needle placed directly into the bladder—may be the preferred method in many cases.
This is especially true when you need a sterile urine sample, such as for culture and sensitivity testing for UTIs. And in general, a cystocentesis will provide more accurate results than a free catch urine sample, since it reduces contamination from cells or pathogens of the skin.
It’s possible to perform a cystocentesis by palpating the bladder or using anatomical landmarks alone. However, an ultrasound can make the process easier by removing the guesswork and allowing you to visualize everything.
Here’s how it works…
How to perform an ultrasound-guided cystocentesis for dogs and cats
Prepare for the procedure.
Use an appropriate size syringe (usually 3ml to 12ml) based on the size of your patient.
Choose a needle size and length based on your patient size. A 22g needle works well for many patients.
Use a towel, trough, or other cushioning to make your patient more comfortable during the procedure. This may help minimize their movement.
Use appropriate patient restraint.
For some dogs and cats, this could mean having a trained team member hold them. For very anxious or fractious patients, this might mean chemical restraint.
Dorsal recumbency is generally the best way to position your patient.
Be sure to clean the area of skin where you’ll be performing the cystocentesis. If needed, consider clipping the fur, too.
Estimate the bladder location.
You’ll use your ultrasound to see the bladder, but anatomical landmarks will give you a good starting point for where to place the probe. Try one of these methods…
Locate the caudal four mammary nipples and mentally draw an ‘X’ between them. The bladder will often be near the cross point of the ‘X’.
Place a small amount of alcohol on the caudal abdomen so it pools. Often, the bladder is located directly under where the alcohol naturally pools on the midline.
Visualize the bladder.
Place your probe onto the caudal abdomen. You should be able to see the urinary bladder on the screen—it’s a fluid-filled structure that has the appearance of a ‘black balloon’ with gray or white walls.
Check for any abnormalities.
You could focus on just doing the cystocentesis. However, while you’re visualizing the bladder, it may help to do a cursory exam (or even a more in-depth evaluation, if indicated) to look for any problems contributing to the patient’s urinary symptoms.
For example, note if you see any thickenings, masses, calculi, or other issues in the urinary bladder.
Obtain the urine sample.
Place the needle directly through the abdominal wall, just in front of the ultrasound probe.
Aim the needle slightly caudally.
You should see the needle on your ultrasound screen. Use this visual to guide you, to be sure you get a good, clean sample rather than aspirating part of the bladder wall.
Prepare your sample for analysis.
Right after the cysto, replace the needle on the syringe with a sterile one.
Then, divide and prepare the sample in a timely manner (the fresher the sample, the better for testing) for any tests you need to perform, whether that’s in-house or at an outside lab.
In many veterinary hospitals, cystocentesis is safely performed several times per day, and complications are very rare. However, as with all medical procedures, some risks exist.
These may include…
Hematuria (usually mild and transient).
Much rarer complications such as bladder injury, leakage of urine into the abdomen, puncture of internal organs or blood vessels, or vagal reactions (retching, panting, hypersalivation, collapse).
Seeding of tumors.
If you suspect your patient has a bladder tumor such as transitional cell carcinoma, it may be best to avoid a cystocentesis. Otherwise, the needle could ‘seed’ the tumor as you withdraw your sample from the bladder, allowing cancer to spread into the abdominal cavity.
An ultrasound may help you to notice abnormalities such as bladder tumors during the procedure, in which case your recommendation to the client may change.
Fortunately for most pets, a cystocentesis is a quick outpatient procedure that provides a lot of valuable information. And many dogs and cats don’t show any side effects at all.
For patients with urinary symptoms, a cystocentesis is often the way to go for the most accurate diagnostic testing results and to get to the bottom of the issue faster for healthy pets and happy clients.
Written by: Dr. Tammy Powell, DVM
Post-Dental Care for Dogs & Cats: Prevent Periodontal Issues
Much attention is focused on the time leading up to and during dental work in dogs and cats, with much attention being placed on the dental procedure itself.
Without education of the pet parent, preventative care can fall to the wayside, leading to continued periodontal problems in the pet.
Dental calculus can form hours after teeth cleaning, thus making the education of the pet parent a vital part of their pet’s dental health.
Properly educating the pet parent about post-dental preventative care entails a recheck visit a week or sooner after the dental, where the pet’s mouth is rechecked, handouts and dental preventative products are introduced to the pet parent, and a demonstration performed to demonstrate proper oral care techniques.
The best way of preventing gum and tooth disease in dogs & cats is to actively brush the pet’s teeth at least 3 to 4 times weekly.
There are some excellent products, including enzymatic toothpaste-like C.E.T. which can break down much of the tartar and debris on the teeth.
During their recheck examination, pet parents can be shown how to brush their pet's teeth using a standard toothbrush, finger brush, and even gauze.
Emphasis should be placed on emphasizing the importance of making the effort to get the habit of home oral care started.
Other products that the pet parent can offer their dog or cat are chewable products such as C.E.T Hygiene chews, Greenies, and other over the counter dental products such as powders, sprays, and gels, as well as water additives.
During the post dental recheck visit, importance should be placed not only on the aforementioned but mentioning diet as well.
Pets eating canned food may be more susceptible to periodontal disease due to the sugars in the food, as well as the wet food sticking to the teeth.
Regular visits to the veterinarian for an oral health exam can give the pet owner an indication of how well they are maintaining the oral health of their pet.
Written by: Dr. Tammy Powell, DVM
What Dental Radiographs Reveal Beneath the Gumline in Pets
When it comes to dentistry, sometimes teeth are like icebergs—there’s a lot going on “below the surface.” In this case, under the gumline.
Unfortunately, the parts of the tooth you can see don’t always tell the whole story.
That’s where dental radiography comes in.
Here are a few situations when dental x-rays could make your client communications easier, help you provide better patient care, and improve your bottom line…
Finding pesky root tips
If you’re extracting a tooth with a fractured root—whether the root splintered prior to the dental procedure or the tip happened to break off during a difficult extraction—you generally want to be sure you’ve removed each and every piece.
In many cases, root tips left behind can lead to infection, pain, or an abscess, plus another procedure to retrieve the piece and an unhappy client.
Radiographs help because you have confirmation that you’ve removed all pieces of the tooth roots.
For extractions, it can be useful to take “before and after” images that clearly document the successful removal of the tooth and its root(s).
Informing owners of the risk of jaw fractures
Sometimes, periodontal disease has caused so much bone loss that it leads to a pathological fracture in the jaw.
Or, the jaw could have so much bone loss that there’s a high risk of iatrogenic jaw fracture during a dental procedure and extraction.
You can probably imagine what could go wrong without radiographs…
When you extract the bad tooth, a jaw fracture can occur if that area of the mandible is already severely compromised due to disease and bone loss. But without radiographic proof of the underlying condition, the client may be inclined to blame your technique, rather than recognizing the severity of their pet’s periodontal disease.
Taking radiographs beforehand helps to set up realistic expectations of risk.
Discovering retained and impacted teeth
Whenever teeth are missing, dental x-rays are a good idea.
Sometimes, below the gumline, you’ll find retained or impacted teeth. Left in place, they could lead to dentigerous cysts or other problems.
Without radiographs, these “hidden” teeth can be difficult to find and treat.
Detecting damage to neighboring teeth
Maybe there’s one tooth that’s obviously bad… But, bone loss and infection have also affected the integrity of the neighboring teeth.
Dental radiographs will help you determine whether or not neighboring teeth are viable. And, the images provide tangible evidence that a neighboring tooth needs to be extracted.
This visual aid can make it easier to show a client exactly what you’re talking about, and help to reinforce your recommendations.
And more…
Dental radiographs can also help you look for oral neoplasias, feline resorptive lesions, tooth root abscesses, and more.
Sometimes this will help to confirm your clinical suspicions based on the patient’s presentation and symptoms. Other times, the findings may come as a surprise—allowing you to treat before the problem becomes worse.
With all the information dental x-rays provide, they can really help you create a thorough treatment plan that covers everything a patient needs during their dental procedure.
Your treatment recommendations can help to improve your dentistry revenue. And, importantly, your dental images can also help you provide excellent patient care and increase client knowledge and compliance.
Ask us about a free demo for your hospital, to see how dental radiography can fit into your practice space and daily appointment flow.
Written by: Dr. Tammy Powell, DVM
Mastering FORLs: X-Ray Insights for Better Dental Procedures
To extract or not to extract that tooth root?
Is a crown amputation all that’s needed?
When it comes to feline odontoclastic resorptive lesions (FORLs), these may be the questions you’re asking yourself.
FORLs can cause loss of the protective surfaces (enamel, cementum, and dentin) of both the crown and the root(s) of a tooth, resulting in pain.
These lesions come in two varieties:
Type 1: Where the root appears radiographically normal.
Type 2: Where the root is radiographically hard to distinguish from the surrounding bone, with loss of visibility of the periodontal ligament space.
As you know, the treatment for these lesions is different—full extraction of the root(s) for Type 1, versus just a crown amputation for Type 2.
Performing a crown amputation and leaving a root in place for Type 1 could result in problems or complications, not to mention continued pain for the patient.
On the other hand, trying to extract the root of a true Type 2 lesion could be a monumental task and a big headache.
So, it’s very important to determine what type of lesion you’re dealing with. Here’s how…
Diagnosing FORLs
Patient presentation:
A client brings their pet to you because of halitosis, food dropping, and occasional jaw chattering.
During the physical exam, you notice bright red, inflamed gums and gingival hyperplasia near one of the mandibular premolars.
You suspect a FORL—and given that FORLs are one of the most common dental problems in cats, you’re probably right.
You suggest a dental procedure, including dental radiographs, a full cleaning, oral exam, and possible extraction. The client agrees with the plan.
The day of the procedure
After the patient is anesthetized, your technician obtains radiographic images of the entire mouth, which takes just a few minutes to perform.
Then, you look at the radiographs in conjunction with your oral exam.
While probing the tooth in question, you feel a rough patch under the gingival hyperplasia, consistent with a resorptive lesion.
The x-ray confirms your diagnosis.
Determining the best treatment plan
In this case, the patient’s tooth is clearly Type 1, with a periodontal ligament space still visible. So, you perform a full extraction.
While evaluating the dental rads, you also notice the premolar on the opposite side is starting to show radiographic evidence of a lesion.
Even though it’s mild, you call the owner and inform them of the likelihood of progression.
To prevent a painful lesion from developing between dentals, the owner decides to go forward with a pre-emptive extraction of that tooth as well.
Documenting the extraction
In addition to being an integral part of your treatment plan decisions, dental radiographs can also help you document that extraction was performed successfully.
A post-procedure x-ray image is a great way to document that there are no root tips left behind.
And, in cases where a crown amputation was indicated, dental rads provide visual proof that this was an appropriate treatment course.
In this way, dental radiographs not only help you to plan and implement a very high quality of medicine—but they also give you peace of mind and are a valuable part of your medical records.
Talking to clients about dental radiographs
Maybe you already know the benefits of dental radiography—but you’re concerned about discussing the additional cost with clients.
Often, it helps to include the x-rays as part of the dental procedure package. List them on the estimate so the client understands the value they are receiving—just don’t itemize the cost of the radiographs separately.
Be sure to adjust the estimate of the dental package accordingly, to cover your costs. And remember, with a monthly payment plan for your dental radiography system, just a couple of dental procedures per month can cover your investment.
Client education also helps. Explain how the results of the radiographs allow you to provide the best possible treatment and reduce the likelihood of future complications.
With clients who want the best for their pets, it’s a win-win for both of you.
Written by: Dr. Tammy Powell, DVM
How to Explain Halitosis Risks to Concerned Pet Owners
Bad breath, or halitosis, is one of those health problems that’s easy for pet parents to overlook.
Sure, it’s inconvenient. Stinky breath can certainly put a damper on a pet owner’s cuddle time or other interactions with their dog or cat.
However, many pet owners don’t realize that halitosis can mean something much worse… such as periodontal disease, or even an internal problem.
As a veterinarian, you know this very well—but it can be a challenge to communicate the dangers lying “under the surface” when it comes to bad breath.
Explaining halitosis to pet parents
The first step is figuring out where the bad breath is coming from, and explaining the potential risks to clients.
Dental problems such as periodontal disease are the most common cause of bad breath in pets.
But sometimes, halitosis begins somewhere in the body other than the mouth.
Possible sources of halitosis include…
Periodontal disease and other dental issues.
A health condition such as kidney disease (an ammonia-like or unpleasant smell) or diabetic ketoacidosis (more of a sweet smell).
Respiratory diseases.
Digestive issues or dietary indiscretions.
Objects (like branches or chicken bones) stuck somewhere in the mouth.
Oral neoplasias.
Certain toxins.
Based on your patient’s history and physical exam, you’ll determine the most likely cause of the bad breath and decide if diagnostic testing is needed.
If the patient in front of you seems otherwise healthy but has apparent terrible dental disease, you can probably assume the smell (or at least, a large portion of the scent) is coming directly from their mouth.
If a dental procedure is indicated, you’ll likely do pre-op bloodwork, which will help confirm that the patient is otherwise healthy.
A recap of periodontal disease
It all starts with plaque, that thin film that forms on teeth due to food and saliva. We get plaque as humans, too, but fortunately, plaque can be removed by tooth brushing.
If not brushed away, plaque hardens into calculus (tartar) within as little as 24-36 hours. Then, it accumulates more and more over time and harbors bacteria. Calculus can’t be removed by toothbrushing alone.
Soon, this calculus (and its resident bacteria) become very irritating to the gums—and they like to grow below the gum line, where it’s harder to observe the process visually. This results in gingivitis, an early stage of periodontal disease (a disease process affecting the structures that hold teeth in place) where the gums become red and inflamed and may bleed.
From here, as the periodontal disease worsens, it creates pockets in the gumline, destruction of the periodontal ligament, and even bone loss in the maxilla and mandible. In severe cases, this bone loss can cause jaw fractures.
This all leads to pain and tooth loss. And, opportunistic bacteria may enter the bloodstream via inflamed gums, traveling to and causing problems in organs such as the heart or kidneys.
Reminding clients of the dangers of periodontal disease can help them understand their pet’s bad breath is true health and quality of life problem—not just an inconvenience.
Evaluating and treating dental and periodontal disease
Your initial pre-op exam will be done while the patient is awake—ideally with the owner present so you can show them what you’re seeing.
However, awake exams don’t allow for a full oral assessment. And, dogs or cats who are painful might not let you get a good look.
So you’ll make a dental cleaning estimate based on your initial exam but explain to the client that the full assessment will be done during the procedure.
This assessment should include dental radiographs. Since much of the disease process starts below the gumline, x-rays are the only way to see the full extent of damage from periodontal disease.
Some patients will just need routine cleaning, while others may need significant dental extractions. And, you can talk to your clients about continuing dental care at home through tooth brushing and dental treats.
By providing this valuable service, you’ll be not only keeping your canine and feline patients in great health—but also increasing the human-animal bond by preventing halitosis from interfering with the quality time between a pet and their owner.
Disclaimer: This article is for general informational purposes only, and not intended as a guide to the medical treatment of any specific animal.
Written by: Dr. Tammy Powell, DVM
The Veterinarian’s Guide to Diagnosing Heart Tumors in Pets
Cancers of the heart are uncommon in dogs and cats. When they do occur, it’s important to differentiate a tumor from other conditions that could cause generalized or focal enlargement of the heart and cardiovascular symptoms.
Which Cancers Occur In Cardiac Tissues?
A cancerous lesion based at the heart could be a primary tumor, or due to metastasis.
Primary tumors that occur at the heart include:
Hemangiosarcomas—the most common heart cancer in dogs, usually occurring at the right atrium. These occur most frequently in larger dogs with longer noses, such as Golder Retrievers, Doberman Pinschers, and German Shepherds.
Chemodectomas, also known as aortic body tumors or heart base tumors. Generally thought to be slow-growing, these tumors occur most commonly in brachycephalic breeds like Boxers, Bulldogs, and Boston Terriers.
Myxomas.
Sarcomas.
Ectopic thyroid tumors.
Lymphoma/lymphosarcoma—the most common heart cancer in cats.
Other cancers are possible, but these are the most commonly diagnosed types. Breeds may vary as noted above, but most pets with tumors of the heart are middle-aged or older.
How Are Heart Tumors Diagnosed?
If slow-growing, tumors near the heart base are often an incidental finding, seen on thoracic radiographs that are taken for another reason.
Other times, diagnostics are pursued because of clinical symptoms—which are often sudden in onset.
Once a mass is large enough to push on the heart and major blood vessels, many cardiovascular symptoms are possible, such as:
Coughing
Ascites
Lethargy
Weakness
Vomiting
Loss of appetite
Difficulty breathing
Collapse
Sudden death
Note: If a dog presents with some of these symptoms, especially sudden weakness and collapse, a quick ultrasound scan may help to identify pericardial effusion and aid in guiding a needle for emergency pericardiocentesis.
Finding Heart Masses Early
As with most cancers and disease processes, discovering a problem earlier rather than later can allow for more treatment options.
General screening radiographs or ultrasound checks—such as with a senior wellness health check—can be a good opportunity to discover heart base tumors before they cause cardiovascular dysfunction and symptoms.
An echocardiogram performed via ultrasound can help to provide more information on the location, size, and invasiveness of the mass.
In some cases, a presumptive diagnosis may be made based on the appearance and location of the mass on an ultrasound study, along with the patient’s signalment. If possible to perform without undue risk, an ultrasound-guided aspirate of the mass can provide more information about which type of tumor is present.
Treatment Options For Cancers Of The Heart
Treatment will be based on the type of neoplasia, how fast the mass is growing, whether metastasis is present, and whether or not the pet is symptomatic.
When a tumor of the heart is diagnosed, a good next step is to screen for metastasis and concurrent conditions via chest x-rays (if not already done), bloodwork, lymph node evaluation, and abdominal ultrasound.
Once a diagnosis is made, treatment options may include:
Periodic monitoring with a cardiologist (especially for slow-growing chemodectomas/heart base tumors) prior to pursuing more invasive treatments.
Surgery to remove the tumor.
Pericardiectomy to remove the pericardium and prevent life-threatening cardiac tamponade or pericardial effusion.
(A pericardiocentesis may be necessary on an emergency basis prior to diagnostics in a pet who presents with acute symptoms. After that, a planned pericardiectomy can help to prevent further emergency episodes of fluid buildup around the heart.)
Chemotherapy, often in conjunction with surgery.
Radiation therapy—either conventional, or via Cyberknife therapy.
Even though cancers of the heart are uncommon in pets, they can be scary to pet owners because of the possibility of sudden onset of serious clinical symptoms (especially with hemangiosarcomas).
By performing diagnostics, referring to specialists as needed, and giving your clients as much information as possible, you can help them make an informed decision for their pet.
Disclaimer: This article is for general informational purposes only, and not intended as a guide to the medical treatment of any specific animal.
Written by: Dr. Tammy Powell, DVM
Vomiting in Cats: Common Causes and Diagnostic Steps
Cats are good at hiding illness and pain. So, for some feline patients, it’s hard to tell what’s behind a bout of vomiting.
A few of the many possible causes include:
Hairballs.
Food sensitivities.
Dietary indiscretion.
Infections or parasites.
Stress.
Pain.
GI foreign bodies.
Inflammatory conditions.
Internal issues such as kidney disease or hyperthyroidism.
Cancer.
Is it serious?
Often, it’s obvious whether the patient needs aggressive treatment right away or just needs a little bit of supportive care and observation at home.
However, other times it’s more difficult to know for sure. Those are the cases that may stay on your mind, making you wonder if the vomiting will continue or even become more severe.
It’s especially nerve-wracking if the patient went home for observation, but you’re concerned they may get worse overnight.
Reaching a diagnosis
Depending on the patient’s signalment, history, and physical exam findings, you’ll recommend the appropriate diagnostic tests.
Bloodwork
Bloodwork is a key factor in determining overall health status, and in establishing a baseline to monitor the patient for improvement or worsening of their condition.
These labs may be especially valuable in senior cats who have lost weight, when kidney disease, hyperthyroidism, or other internal medicine issues may be what comes to mind as the most likely diagnosis.
Imaging with x-rays and ultrasound
For some patients—especially if the vomiting is severe, or if you feel something abnormal on abdominal palpation—imaging may be needed right away. For patients with milder signs, you may decide to hold off on imaging at the first visit, but recommend the client bring their cat back if symptoms don’t improve.
And even if an obvious abnormality is noted on bloodwork (such as elevated thyroid hormone), imaging is still a good idea to rule out concurrent conditions, and to establish a baseline to compare any changes that show up on future imaging tests.
Either way, when it comes to imaging, radiographs are a good place to start.
Radiographs give you a good overview of what’s going on inside the abdomen. You can look for masses, abnormal-looking organs, constipation, bladder issues, pyometra, signs of a GI obstruction, and much more.
However, sometimes more information is needed. Often, x-rays and ultrasound work well together to give you the full picture.
Ultrasound gives you additional clues about soft tissue structures, including:
Differentiating a mass (size, what the borders look like, texture, thickness, etc.) from surrounding normal soft tissues. Silhouetting may make this interpretation challenging on x-ray images.
Viewing bladder stones that aren’t radiopaque.
Looking at small structures that are hard to see on x-rays, such as the adrenal glands.
Inflammation of the GI tract or other internal organs.
Finding evidence of a GI obstruction when it’s not obvious on radiographs (or, ruling out an obstruction—which may help you worry less if you decide to send the patient home for monitoring).
The list goes on, but the point is, x-rays and ultrasound can complement each other to give you the information you need, which can help you confidently diagnosis the mysterious vomiting cat.
Additional tests
Sometimes additional tests—for example, biopsies and infectious disease testing—may be needed to reach a diagnosis.
However, bloodwork, x-rays, and ultrasound are a great place to start. And often, these modalities will need to be completed prior to other modalities such as surgically obtained biopsies.
Lifestyle changes and monitoring
If the vomiting is due to a factor such as stress or hairballs, this may require a simple lifestyle change like providing Feliway diffusers and adding mental enrichment at home, or changing to a special diet.
But even in these cases, it’s good to rule out other, treatable medical causes—so a medical workup with diagnostic tests may still be recommended.
Keeping the vomiting at bay
If you have a patient with a chronic condition, you may recommend repeating the bloodwork, x-rays, and ultrasound at regular intervals.
A wellness checkup package that includes testing may be a good option for many patients—especially seniors. The wellness tests can be offered at checkups before the patient ever becomes ill, which gives you a great baseline for comparison with future test results.
Even though cats may not like to show symptoms of illness until a disease has progressed, wellness bloodwork and imaging (x-rays and ultrasound) can help to catch abnormalities early on, when the chances for treatment are better.
Disclaimer: This article is for general informational purposes only, and not intended as a guide to the medical treatment of any specific animal.
Written by: Dr. Tammy Powell, DVM