10 Steps To Complete Dental Cleaning Procedures In Pets
Perform a pre-anesthetic checklist, including patient history, exam, lab work, chest X-rays, and prophylactic medications, especially for senior patients.
Ensure all equipment is functioning properly and that all essential instruments are available and sanitized. Ensure the CPR plan and CPR medications are in place, as well as resuscitation status for each patient.
Provide a safe heat source such as a warm air blanket.
Continually check the patient by placing your hand directly on the patient under the heat source. Include this step on your anesthesia monitoring sheet.
Ensure the patient is warm during the pre-anesthetic phase where a patient’s body temperature can lower.
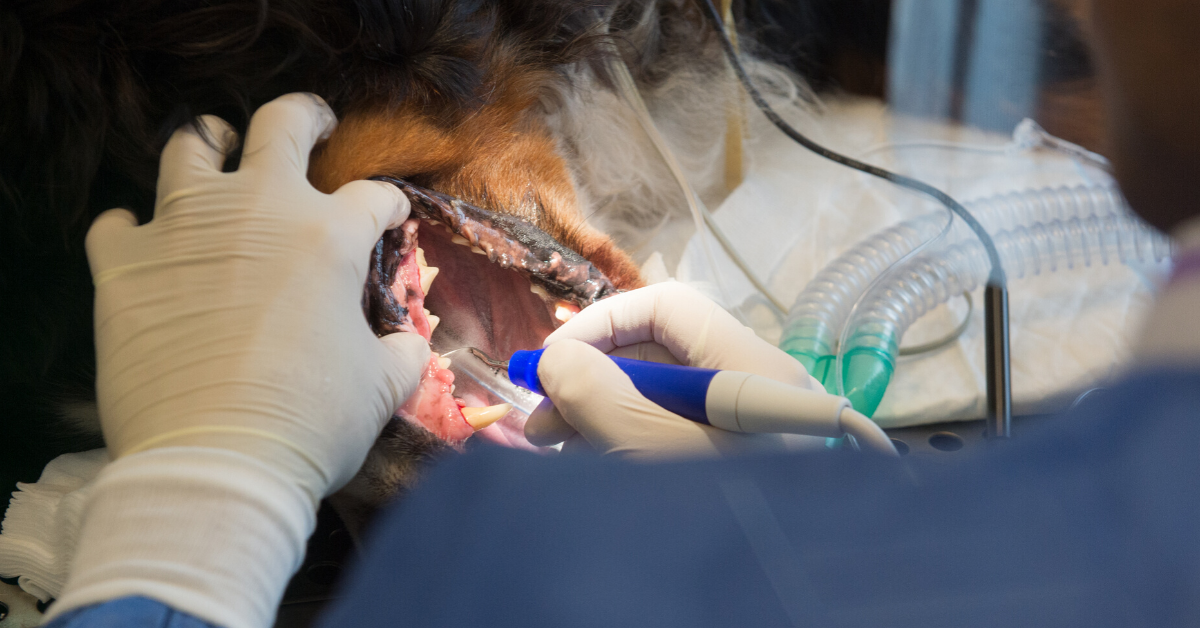
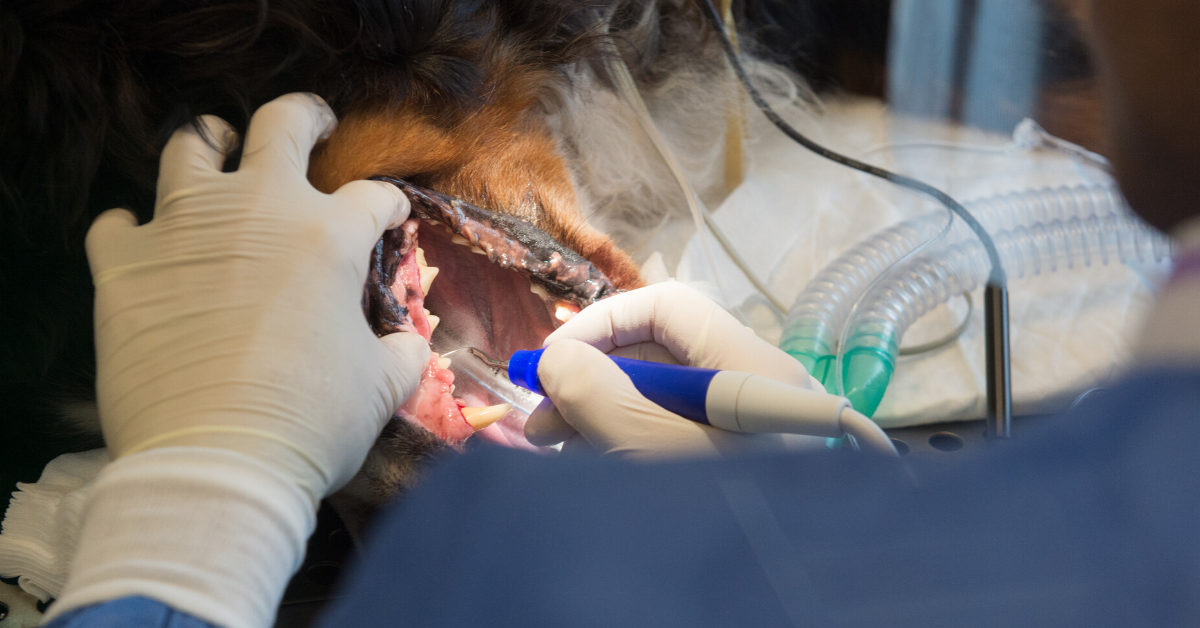
1. During the onset of anesthesia while intubating, use caution when handling the tongue, ensuring it is not pulled forcefully. Gently place the patient in position – note; placing a pet on their back during the entire procedure minimizes anesthesia time and is an effective and expeditious way to perform a dental.
Ensure the tracheal tube is adequately inflated, and an aspiration guard or gauze is in place. Consider the use of intraoral suction to prevent aspiration of water and debris during the procedure.
Continually replace gauze as it becomes saturated with water. Continually check the tracheal tube during the procedure as it may need adjusting depending on the depth of anesthesia and tracheal relaxation
2. While under anesthesia, take before and after photographs of all areas of the mouth to show the pet parent, as well as keep for documentation in the medical record.
3. Begin by irrigating the pet’s mouth with a dilute Veterinary Oral Health Council approved Chlorhexidine based rinse such as CET. Evaluate the oral cavity, and remove obvious calculus at this time to expose gingiva and soft tissues.
4. Perform intraoral regional nerve blocks prior to probing the teeth and gingival tissues, as this procedure may cause pain in the anesthetized patient, requiring a deeper plane of anesthesia.
5. Thoroughly probe and chart each tooth, and perform full-mouth radiographs
6. Clean the teeth, perform extractions, and required orthodontic procedures needed. Ensure hand scalers and a curette are employed to remove subgingival calculus, particularly where periodontal pockets have been identified.
7. Thoroughly irrigate and lavage away oral debris.
8. Polish all surfaces of each tooth and subgingival areas thoroughly and carefully.
9. Rinse the mouth and each tooth with air and water and ensure all debris is removed from the tongue. Take post-procedure photographs.
10. Finally, apply a plaque prevention gel or dental sealant
Recover the patient quietly and employ pain management and anti-inflammatory medication. The post-anesthetic patient should be monitored closely post-surgically.
Written by: Dr. Tammy Powell, DVM
Advanced Veterinary Dentistry: The Role of Digital X-Rays
Veterinary dentistry has become advanced over recent years, particularly with the advent of oral dental radiographs.
The idea of regular dental care for our pets is new to many pet owners who are beginning to realize the importance of regular exams, teeth cleaning, and oral radiographs.
Practice standards are changing, and pet dentistry has become sophisticated and cutting edge. Similar to when humans have an oral examination and teeth cleaning, the dentist will request radiographs to check for underlying problems or concerns.
The same should be expected for pets when they go to the veterinarian for teeth cleaning. Dental radiology is at the forefront of ever changing veterinary practice standards.
With most of a tooth lying below the gum surface (think of an Iceberg), problems cannot be appreciated until a radiograph is taken and reviewed.
It is virtually impossible to practice veterinary dentistry without dental radiographs, which allow visualization of tooth roots, bone, and surrounding structures not visible otherwise.
Dental radiographs today are not taken with the conventional x-ray unit seen at most veterinary clinics.
Today’s advanced dental x-ray units give exceptional detail and clarity. Dental x-rays are easy to use and typically located adjacent to the patient. They are made using small radiographic films or digital sensors placed inside the patient’s mouth, and can generally be accomplished within 10 or 15 minutes when performed by an experienced and trained technician.
Typically 6-8 images are taken during a routine pet dental cleaning. The radiation risk to the patient from dental radiographs is minimal and outweighs the risk of missing underlying dental problems.
Dental radiographs should be performed early to establish a baseline for future comparison.
Ideally, this can be accomplished at the same time puppies and kittens are undergoing routine spay and neutering and should be performed under anesthesia to effectively diagnose and assist in treating a patient with periodontal disease or underlying pathologic complications.
Anesthesia is important to obtain dental radiographs because the sensor or films must be placed in the pet’s mouth, which would be difficult to accomplish awake.
Studies show that without dental radiographs, up to 75% percent of significant dental problems are missed in pets undergoing routine teeth cleaning.
In addition, the AAHA (American Animal Hospitals Association) Dental Care Guidelines for Dogs and Cats state that preoperative and postoperative dental radiographs are mandated for all tooth extractions.
Dental radiographs taken prior to extractions ensure that a procedure can be properly planned and that no underlying issues such as developmental defects surprise the individual performing the extractions.
Post extraction radiographs ensure that all root fragments are removed and that no inadvertent damage was caused.
A pet can be left in discomfort for years if problems are missed during a dental.
Pets showing dental problems may avoid hard food, have red or bleeding gums, bad breath, have problems picking up and dropping food, make noises when they yawn, chew on one side of the mouth, excessively sneeze, express facial discomfort by pawing at the mouth, excessively salivate, exhibit ropey drool, and more.
Any pet exhibiting these signs should have a dental with oral radiographs to allow the veterinarian to make an accurate diagnosis. Once a diagnosis has been established, the proper treatment plan can then be instituted. Without dental radiographs, an accurate diagnosis is not possible, and pets may needlessly suffer.
Indications for dental radiographs in pets:
Periodontal Disease and Extractions: Radiographs help to determine a treatment plan, identify retained tooth roots, follow each pet’s dental progression as they age, and to assist the operator during extractions to avoid potential injury such as jaw fractures.
Trauma: Identify a fracture or foreign body such as shrapnel or other material.
Defects and Variations in Tooth Density: Identify cavities or resorption lesions in cats.
Endodontic Issues: Determine if a tooth requires a root canal.
Developmental Defects/Anomalies: Detection of supernumerary teeth, missing teeth or teeth that have failed to erupt.
Swellings, Cysts, Tumors: Help determine the source of facial swelling and pain.
Advanced procedures: Pets receiving advanced procedures such as crowns, braces, jaw fracture repair, oral tumor removal.
With modern medical advances in veterinary dentistry, dental radiographs should always be implemented in the complete periodontal exam and treatment of pets undergoing dental cleaning with extractions.
It is otherwise not possible to provide good quality dental care and documentation without utilizing radiographs.
Dental radiography is the number one diagnostic tool in the practice of complete pet dentistry.
Written by: Dr. Tammy Powell, DVM
Veterinary Solutions for Pet Oral Health and Periodontal Care
Periodontal disease is an inflammation and infection in the gums around your pet’s teeth caused by bacteria which adheres to a sticky substance called plaque.
Left untreated, this turns into hard tarter (calculus), which builds up under the gum line and surface of the teeth. Periodontal disease is characterized as gingivitis and periodontitis. Gingivitis is inflammation or reddening of the gums (gingiva), and periodontitis is loss of bone and soft tissue around the teeth leading to non-salvageable loose teeth, malodorous breath, and potential jaw fractures.
This is a very common issue in pets. Periodontal disease is a painful disease and is thought now to be an epidemic. When it starts, periodontal disease shows no outward signs and symptoms, and many pet owners are unaware of the problem in the pet’s mouth until the disease has advanced.
Some symptoms of severe periodontal disease include:
Pawing at the mouth
Red or bleeding gums with bad breath
Loose teeth
Problems picking up food and dropping food
A swelling on the muzzle near the eye caused by an abscessed tooth root (often pet owners think this is a bite).
Making noises when a pet eats or yawns
Head shyness
Bloody or ropey saliva seen in water or toys
Chewing on one side of the mouth
Sneezing or nasal discharge – the nasal cavity can become infected
All breeds and sizes of dogs and cats are at risk of periodontal disease.
This disease not only affects the mouth, but bacteria entering the bloodstream affects the immune system. The risk of associated health complications can be reduced by proper dental hygiene.
Multiple health problems linked to periodontal disease include internal organ problems such as heart and lung disease, liver and kidney disease, bladder infections, pancreatitis, weight loss, and behavioral issues such as biting or suddenly becoming isolated, among others.
Periodontal disease can almost always be prevented or minimized with a combination of home dental care and veterinary dental cleaning.
Once tartar is formed, it cannot be brushed off with a toothbrush. Routine daily teeth brushing can remove the sticky plaque, however, not the tarter.
Trying to brush the teeth when the mouth is inflamed and teeth are loose and Infected will cause your pet to resent brushing and oral care.
Once your pet has undergone a thorough dental and the mouth heals, daily brushing will prevent further dental disease.
A deep thorough subgingival cleaning under the gum line is important and necessary to remove the tarter and infected teeth and must be performed under anesthesia. Non-anesthesia teeth cleaning is solely cosmetic and does not address the source of the problem laying under the gum line. It is important to start brushing as a puppy and kitten and make this a daily routine.
As long as the surfaces of the teeth are cleaned frequently, the gums will stay healthy. The sooner you start to clean your pet’s teeth, the less likely your pet will need extractions.
Periodontal disease prevention includes:
A veterinary examination of your pet’s mouth and teeth at all ages is important. Early detection of problems such as teeth crowding and retained baby teeth can be addressed and resolved.
On-going plaque and tarter control are key to the prevention of oral disease. Teeth brushing daily is the most important way to prevent gum disease. Many pet owners are concerned that they will not be able to perform this task. Many dogs and cats will actually enjoy the daily interaction and like the taste of the dental products.
Look for products with the Veterinary Oral Health Council (VOHC) seal of approval such as toothpaste, oral rinse, and water additives, made to keep your pet’s teeth clean and the gums and bone healthy.
Canned food tends to stick to the teeth more than dry food. Look for dental diets that help pet’s teeth as they chew. A good quality dry kibble works best. Your veterinarian has information about dental based diets.
Offer Dental treats and chews. This is a good way to help prevent periodontal disease in pets. Look for bendable, soft toys and treats and avoid hard treats such as antlers. Use rope toys, rubber balls, and rubber toys where you can hide treats.
Oral health is fundamental to the general health of pets and essential to preventing periodontal disease. Teaching the pet owners that your animal hospital serves to get into the habit of daily dental care with their pet allows bonding time, and can be fun and looked at as “treat time” for their pet.
Written by: Dr. Tammy Powell, DVM
Post-Dental Care for Dogs & Cats: Prevent Periodontal Issues
Much attention is focused on the time leading up to and during dental work in dogs and cats, with much attention being placed on the dental procedure itself.
Without education of the pet parent, preventative care can fall to the wayside, leading to continued periodontal problems in the pet.
Dental calculus can form hours after teeth cleaning, thus making the education of the pet parent a vital part of their pet’s dental health.
Properly educating the pet parent about post-dental preventative care entails a recheck visit a week or sooner after the dental, where the pet’s mouth is rechecked, handouts and dental preventative products are introduced to the pet parent, and a demonstration performed to demonstrate proper oral care techniques.
The best way of preventing gum and tooth disease in dogs & cats is to actively brush the pet’s teeth at least 3 to 4 times weekly.
There are some excellent products, including enzymatic toothpaste-like C.E.T. which can break down much of the tartar and debris on the teeth.
During their recheck examination, pet parents can be shown how to brush their pet's teeth using a standard toothbrush, finger brush, and even gauze.
Emphasis should be placed on emphasizing the importance of making the effort to get the habit of home oral care started.
Other products that the pet parent can offer their dog or cat are chewable products such as C.E.T Hygiene chews, Greenies, and other over the counter dental products such as powders, sprays, and gels, as well as water additives.
During the post dental recheck visit, importance should be placed not only on the aforementioned but mentioning diet as well.
Pets eating canned food may be more susceptible to periodontal disease due to the sugars in the food, as well as the wet food sticking to the teeth.
Regular visits to the veterinarian for an oral health exam can give the pet owner an indication of how well they are maintaining the oral health of their pet.
Written by: Dr. Tammy Powell, DVM
What Dental Radiographs Reveal Beneath the Gumline in Pets
When it comes to dentistry, sometimes teeth are like icebergs—there’s a lot going on “below the surface.” In this case, under the gumline.
Unfortunately, the parts of the tooth you can see don’t always tell the whole story.
That’s where dental radiography comes in.
Here are a few situations when dental x-rays could make your client communications easier, help you provide better patient care, and improve your bottom line…
Finding pesky root tips
If you’re extracting a tooth with a fractured root—whether the root splintered prior to the dental procedure or the tip happened to break off during a difficult extraction—you generally want to be sure you’ve removed each and every piece.
In many cases, root tips left behind can lead to infection, pain, or an abscess, plus another procedure to retrieve the piece and an unhappy client.
Radiographs help because you have confirmation that you’ve removed all pieces of the tooth roots.
For extractions, it can be useful to take “before and after” images that clearly document the successful removal of the tooth and its root(s).
Informing owners of the risk of jaw fractures
Sometimes, periodontal disease has caused so much bone loss that it leads to a pathological fracture in the jaw.
Or, the jaw could have so much bone loss that there’s a high risk of iatrogenic jaw fracture during a dental procedure and extraction.
You can probably imagine what could go wrong without radiographs…
When you extract the bad tooth, a jaw fracture can occur if that area of the mandible is already severely compromised due to disease and bone loss. But without radiographic proof of the underlying condition, the client may be inclined to blame your technique, rather than recognizing the severity of their pet’s periodontal disease.
Taking radiographs beforehand helps to set up realistic expectations of risk.
Discovering retained and impacted teeth
Whenever teeth are missing, dental x-rays are a good idea.
Sometimes, below the gumline, you’ll find retained or impacted teeth. Left in place, they could lead to dentigerous cysts or other problems.
Without radiographs, these “hidden” teeth can be difficult to find and treat.
Detecting damage to neighboring teeth
Maybe there’s one tooth that’s obviously bad… But, bone loss and infection have also affected the integrity of the neighboring teeth.
Dental radiographs will help you determine whether or not neighboring teeth are viable. And, the images provide tangible evidence that a neighboring tooth needs to be extracted.
This visual aid can make it easier to show a client exactly what you’re talking about, and help to reinforce your recommendations.
And more…
Dental radiographs can also help you look for oral neoplasias, feline resorptive lesions, tooth root abscesses, and more.
Sometimes this will help to confirm your clinical suspicions based on the patient’s presentation and symptoms. Other times, the findings may come as a surprise—allowing you to treat before the problem becomes worse.
With all the information dental x-rays provide, they can really help you create a thorough treatment plan that covers everything a patient needs during their dental procedure.
Your treatment recommendations can help to improve your dentistry revenue. And, importantly, your dental images can also help you provide excellent patient care and increase client knowledge and compliance.
Ask us about a free demo for your hospital, to see how dental radiography can fit into your practice space and daily appointment flow.
Written by: Dr. Tammy Powell, DVM
How to Explain Halitosis Risks to Concerned Pet Owners
Bad breath, or halitosis, is one of those health problems that’s easy for pet parents to overlook.
Sure, it’s inconvenient. Stinky breath can certainly put a damper on a pet owner’s cuddle time or other interactions with their dog or cat.
However, many pet owners don’t realize that halitosis can mean something much worse… such as periodontal disease, or even an internal problem.
As a veterinarian, you know this very well—but it can be a challenge to communicate the dangers lying “under the surface” when it comes to bad breath.
Explaining halitosis to pet parents
The first step is figuring out where the bad breath is coming from, and explaining the potential risks to clients.
Dental problems such as periodontal disease are the most common cause of bad breath in pets.
But sometimes, halitosis begins somewhere in the body other than the mouth.
Possible sources of halitosis include…
Periodontal disease and other dental issues.
A health condition such as kidney disease (an ammonia-like or unpleasant smell) or diabetic ketoacidosis (more of a sweet smell).
Respiratory diseases.
Digestive issues or dietary indiscretions.
Objects (like branches or chicken bones) stuck somewhere in the mouth.
Oral neoplasias.
Certain toxins.
Based on your patient’s history and physical exam, you’ll determine the most likely cause of the bad breath and decide if diagnostic testing is needed.
If the patient in front of you seems otherwise healthy but has apparent terrible dental disease, you can probably assume the smell (or at least, a large portion of the scent) is coming directly from their mouth.
If a dental procedure is indicated, you’ll likely do pre-op bloodwork, which will help confirm that the patient is otherwise healthy.
A recap of periodontal disease
It all starts with plaque, that thin film that forms on teeth due to food and saliva. We get plaque as humans, too, but fortunately, plaque can be removed by tooth brushing.
If not brushed away, plaque hardens into calculus (tartar) within as little as 24-36 hours. Then, it accumulates more and more over time and harbors bacteria. Calculus can’t be removed by toothbrushing alone.
Soon, this calculus (and its resident bacteria) become very irritating to the gums—and they like to grow below the gum line, where it’s harder to observe the process visually. This results in gingivitis, an early stage of periodontal disease (a disease process affecting the structures that hold teeth in place) where the gums become red and inflamed and may bleed.
From here, as the periodontal disease worsens, it creates pockets in the gumline, destruction of the periodontal ligament, and even bone loss in the maxilla and mandible. In severe cases, this bone loss can cause jaw fractures.
This all leads to pain and tooth loss. And, opportunistic bacteria may enter the bloodstream via inflamed gums, traveling to and causing problems in organs such as the heart or kidneys.
Reminding clients of the dangers of periodontal disease can help them understand their pet’s bad breath is true health and quality of life problem—not just an inconvenience.
Evaluating and treating dental and periodontal disease
Your initial pre-op exam will be done while the patient is awake—ideally with the owner present so you can show them what you’re seeing.
However, awake exams don’t allow for a full oral assessment. And, dogs or cats who are painful might not let you get a good look.
So you’ll make a dental cleaning estimate based on your initial exam but explain to the client that the full assessment will be done during the procedure.
This assessment should include dental radiographs. Since much of the disease process starts below the gumline, x-rays are the only way to see the full extent of damage from periodontal disease.
Some patients will just need routine cleaning, while others may need significant dental extractions. And, you can talk to your clients about continuing dental care at home through tooth brushing and dental treats.
By providing this valuable service, you’ll be not only keeping your canine and feline patients in great health—but also increasing the human-animal bond by preventing halitosis from interfering with the quality time between a pet and their owner.
Disclaimer: This article is for general informational purposes only, and not intended as a guide to the medical treatment of any specific animal.
Written by: Dr. Tammy Powell, DVM
Vomiting in Cats: Common Causes and Diagnostic Steps
Cats are good at hiding illness and pain. So, for some feline patients, it’s hard to tell what’s behind a bout of vomiting.
A few of the many possible causes include:
Hairballs.
Food sensitivities.
Dietary indiscretion.
Infections or parasites.
Stress.
Pain.
GI foreign bodies.
Inflammatory conditions.
Internal issues such as kidney disease or hyperthyroidism.
Cancer.
Is it serious?
Often, it’s obvious whether the patient needs aggressive treatment right away or just needs a little bit of supportive care and observation at home.
However, other times it’s more difficult to know for sure. Those are the cases that may stay on your mind, making you wonder if the vomiting will continue or even become more severe.
It’s especially nerve-wracking if the patient went home for observation, but you’re concerned they may get worse overnight.
Reaching a diagnosis
Depending on the patient’s signalment, history, and physical exam findings, you’ll recommend the appropriate diagnostic tests.
Bloodwork
Bloodwork is a key factor in determining overall health status, and in establishing a baseline to monitor the patient for improvement or worsening of their condition.
These labs may be especially valuable in senior cats who have lost weight, when kidney disease, hyperthyroidism, or other internal medicine issues may be what comes to mind as the most likely diagnosis.
Imaging with x-rays and ultrasound
For some patients—especially if the vomiting is severe, or if you feel something abnormal on abdominal palpation—imaging may be needed right away. For patients with milder signs, you may decide to hold off on imaging at the first visit, but recommend the client bring their cat back if symptoms don’t improve.
And even if an obvious abnormality is noted on bloodwork (such as elevated thyroid hormone), imaging is still a good idea to rule out concurrent conditions, and to establish a baseline to compare any changes that show up on future imaging tests.
Either way, when it comes to imaging, radiographs are a good place to start.
Radiographs give you a good overview of what’s going on inside the abdomen. You can look for masses, abnormal-looking organs, constipation, bladder issues, pyometra, signs of a GI obstruction, and much more.
However, sometimes more information is needed. Often, x-rays and ultrasound work well together to give you the full picture.
Ultrasound gives you additional clues about soft tissue structures, including:
Differentiating a mass (size, what the borders look like, texture, thickness, etc.) from surrounding normal soft tissues. Silhouetting may make this interpretation challenging on x-ray images.
Viewing bladder stones that aren’t radiopaque.
Looking at small structures that are hard to see on x-rays, such as the adrenal glands.
Inflammation of the GI tract or other internal organs.
Finding evidence of a GI obstruction when it’s not obvious on radiographs (or, ruling out an obstruction—which may help you worry less if you decide to send the patient home for monitoring).
The list goes on, but the point is, x-rays and ultrasound can complement each other to give you the information you need, which can help you confidently diagnosis the mysterious vomiting cat.
Additional tests
Sometimes additional tests—for example, biopsies and infectious disease testing—may be needed to reach a diagnosis.
However, bloodwork, x-rays, and ultrasound are a great place to start. And often, these modalities will need to be completed prior to other modalities such as surgically obtained biopsies.
Lifestyle changes and monitoring
If the vomiting is due to a factor such as stress or hairballs, this may require a simple lifestyle change like providing Feliway diffusers and adding mental enrichment at home, or changing to a special diet.
But even in these cases, it’s good to rule out other, treatable medical causes—so a medical workup with diagnostic tests may still be recommended.
Keeping the vomiting at bay
If you have a patient with a chronic condition, you may recommend repeating the bloodwork, x-rays, and ultrasound at regular intervals.
A wellness checkup package that includes testing may be a good option for many patients—especially seniors. The wellness tests can be offered at checkups before the patient ever becomes ill, which gives you a great baseline for comparison with future test results.
Even though cats may not like to show symptoms of illness until a disease has progressed, wellness bloodwork and imaging (x-rays and ultrasound) can help to catch abnormalities early on, when the chances for treatment are better.
Disclaimer: This article is for general informational purposes only, and not intended as a guide to the medical treatment of any specific animal.
Written by: Dr. Tammy Powell, DVM
Dental X-Rays: Tips for Accurate Vet Imaging Success
When it comes to evaluating a pet’s teeth, dental x-rays are the best way to see what’s happening “under the surface.” That is, under the gumline.
Dental radiographs help you obtain a full picture of tooth roots, evaluate for periodontal disease and damage, differentiate between different types of FORLs, and look for any other defects that may not be visible with your eyes alone.
Even though the value of dental radiographs (to both your patients and your practice) is hard to deny, there can be a learning curve when your team first begins to use them.
This is important, because in order for your x-ray images to be diagnostic, they need to be good quality.
Fortunately, with practice, dental x-rays become simple and routine—a process your team can quickly replicate for each patient.
Establishing a Dental X-Ray Routine
To make the dental radiograph process easy for you and your team—and as quick as possible for your patients—it’s best to establish a repeatable routine.
This means taking the same shots, in the same order, each time.
You may need a larger number of views depending on the patient’s size and the angle of their mouth, but in general you can start in the same place each time and move through your views systematically until images of all teeth and their roots are captured.
Use your digital software to set up the views in the order you prefer.
Once you establish a routine, it will only take a few minutes to shoot all views for a small patient. And large dogs should take a maximum of 15-20 minutes.
Positioning the Patient
Your patients will be under general anesthesia for their dental procedure, including dental x-rays.
After intubation, leave the patient in sternal recumbency, and simply place a towel under their chin to keep their maxilla parallel to the table. Then obtain your views of the maxillary teeth.
When you finish the views of the maxilla, move the patient to dorsal recumbency, this time using a towel or other prop under their neck to keep the mandible parallel to the table as you obtain your views of the mandibular teeth.
You can use a trough or sandbags to stabilize the patient and keep them from tilting to the side, if needed.
Adjust this plan if you find that another method better suits your needs. For example, you may find that lateral recumbency works best for you for some views.
Whatever system you choose, we recommend repeating the same steps each time and using a method that minimizes the number of times you need to move the patient.
Sensor or Film Placement
Select the right size sensor or film for your patient. For most veterinary patients, this would be either a size 2 (for small dogs and cats, or views focusing on a single tooth) or a size 4 (for large dogs, or for full-mouth/whole quadrant radiographic views).
Whether you’re using a sensor for digital x-rays, or regular dental film, placement is important to ensure you can see all of each tooth root. Remember the roots are much longer than the crowns (twice as long with canine teeth), so position your sensor accordingly.
Finally, determine which side of the sensor or film should be positioned toward the x-ray beam. This may be indicated by a small dot or “dimple” on films. If you have a digital sensor, the cord side should face away from the tube and the cord should exit the front of the patient’s mouth.
Beam Placement
A parallel angle is used for the mandibular premolar and molar teeth. For many pets, this part of the mouth allows the sensor to be placed parallel to the teeth, and the beam to be shot straight forward (perpendicular) into the sensor.
The rest of the mouth, however, prevents this placement (the palate and mandibular symphysis get in the way). So, you’ll need to use a bisecting angle for the rest of your shots (and possibly for the rostral mandibular premolars).
A bisecting angle might seem complicated, but it’s important—choosing the correct angle prevents distortion (lengthening or shortening of the tooth root in your image).
Here is how to determine the bisecting angle:
Position the sensor within the mouth behind the teeth you want to x-ray, as if the patient is biting on it (use gauze or other aids to hold the mouth open so there is no pressure from the teeth that could damage the sensor).
Estimate the angle between the tooth root and the plate.
Divide this angle in half, and draw an imaginary line with your mind.
Position the x-ray beam perpendicular (at a right angle, or 90 degrees) to this line you’ve just imagined.
If the tooth root is too long on your image, raise the angle of the tube relative to the sensor. If the root is too short, lower the angle of the beam (move it more parallel toward the sensor).
Developing a Simplified Technique
Using a simplified technique can allow you to skip the bisecting angle measurement. For example, one described technique uses just three angles for all oral views…
90 degrees for mandibular molars/premolars.
70 degrees for maxillary molars/premolars.
45 degrees for canines and incisors.
Since you can position these angles on your tube head without measuring (many units have predetermined angles marked by the tube head), this makes positioning much easier and faster for you and your staff.
Exceptions, Views of Specific Teeth, and Further Training
These guidelines are a good starting point for many patients. But, you may find you need to adjust your views to accommodate certain dogs and cats, depending on the shape of their mouth and tooth roots.
Cats in particular may need steeper angles than dogs to minimize interference from the zygomatic arch. And some patients will have tooth roots that curve significantly.
For all of these reasons, and for the benefit of hands-on experience, it helps to schedule a demo of your equipment, or to find an in-person training opportunity for your staff. That way, you can maximize your return on investment by using your dental radiography unit to its fullest potential.
Any time spent developing the proper technique for positioning will be well worth it, as you’ll be able to quickly take views that aid your treatment decisions and deliver value to your clients.
Disclaimer: This article is for general informational purposes only, and not intended as a guide to the medical treatment of any specific animal.
Written by: Dr. Tammy Powell, DVM
Essential Tips for Feline Dental Health: Best Practices
As a veterinarian, you already know how important dental health is to your patients—and you also know that dental health concerns can vary by species.
Today, we’ll be covering some tips for dental care in cats, both before and after the dental procedure.
Knowing Your Way Around a Cat’s Mouth
Quick—how many teeth should an adult cat have?
Clients often ask questions like this. A timely, confident answer will help inspire confidence when they leave their pet with you for oral care.
Plus, knowing the normal dental formula for each species serves an important purpose DURING a dental procedure.
For example, it helps a veterinarian or vet tech easily determine whether or not there are any missing teeth—a discovery that could prompt further exploration and potentially diagnose a problem that needs to be addressed.
Similarly, when performing extractions, it’s important to know how many roots the tooth has, to ensure no root tips get left behind. Knowing the approximate length and direction of each root will also help a vet extract the tooth more efficiently.
Know the Most Common Issues to Look For
Of course, dental tartar and periodontal disease are common concerns in both dogs and cats. But each species also carries their own unique dental problems that occur commonly.
For example, FORLs/resorptive lesions are fairly common in cats, but not so much in dogs. Felines are also more prone to certain inflammatory conditions such as stomatitis.
While it’s important to keep a look out for anything that could be part of a disease process, knowing the common issues in each species could help a vet pick up on subtle or early changes.
Also, be aware of normal structures that could be confused for a mass or lesion—such as the lingual molar salivary gland in cats.
Dental Radiographs: Why, When, and How
The WHY is simple: Dental x-rays are important because they allow a veterinarian to see the whole picture of a pet’s dental health—which frequently includes problems brewing below the gumline.
But, WHEN and HOW should dental x-rays be performed?
Many experts recommend taking a full set of dental radiographs immediately after anesthesia induction. Usually, this task is performed by a skilled vet tech or nurse, along with anesthesia monitoring.
It’s worthwhile to invest in training for this important skill. Consider sending team members to a conference or course, or asking the company that sold the dental x-ray equipment if they offer training. And setting up a standard technique (performing the views in the same order each time) can improve efficiency.
Performing radiographs prior to the cleaning gives the vet a chance to review the radiographs. These findings, along with a visual assessment of the patient’s mouth (including charting), gives a lot of information to support a call to the owner, if needed for additional treatments.
For routine cleanings, this may be all that is needed. But for patients who are receiving extractions or more advanced procedures, it’s beneficial to perform post-op dental x-rays. This confirms that everything was done properly and safely, in case any new concerns arise later.
Tips for Cleaning a Cat’s Teeth During a Dental Procedure
After charting is done, the typical dental procedure consists of scaling and polishing.
Scaling of the enamel can be done with an ultrasonic/and or hand scaler, while curettes (sometimes in combination with a specialized, “periodontal tip” on the ultrasonic scaler) are used to clean below the gumline.
Polishing is performed using a low-speed handpiece, usually with disposable prophy angles and fine-grit prophy paste.
Dental extractions may be done at the point during the procedure that works best for that patient’s needs and the veterinarian’s preference. For example, it may make sense to pull very loose teeth prior to cleaning (no point in spending time cleaning a tooth that is about to fall out), while more complicated extractions might be performed further into the procedure.
Here are a few tips for dental cleaning:
Make sure to stock the right size tools (scalers, etc.) in the practice, which means a range of sizes if you see everything from cats to large dogs. Smaller tools for cats allow for getting into crevices and cleaning more efficiently.
Use time limits to avoid overheating of the teeth, i.e. no more than 10 seconds at a time on any tooth with the ultrasonic scaler, or 5 seconds with the polisher.
In cats, due to the small size and shape of their skull, the eye sits very close to the maxillary teeth. Therefore, be careful while probing or cleaning deep periodontal pockets in that area (not to mention during nerve blocks or extractions) to avoid traumatic injuries to the eye.
Due to the prevalence of periodontal disease, and the abundance of oral and dental diseases that can occur in cats, there’s no doubt that dental health is important for their overall health and comfort.
Client expectations are evolving. Many devoted pet owners research dental procedures online and expect a high level of care for their cat’s oral health needs.
By investing in dentistry—and then communicating the value of each step to their clients—a veterinary practice can bring in income while providing excellent care to their feline patients.
Written by: Dr. Tammy Powell, DVM
The Ultimate Guide to Veterinary Dental Cleaning Stations
A comprehensive oral health assessment and treatment (COHAT), also known as a veterinary dental procedure, is an important consideration for any pet’s long-term health.
Keeping the mouth healthy helps protect a dog or cat’s teeth and contributes to a pet’s overall wellbeing. And, it can be a source of revenue for the veterinary practice.
Here are some of the common components of a dental cleaning station, and the roles they play during a COHAT.
The Equipment Needed for Scaling and Polishing
Even for pets who need significant extractions, the dental procedure typically also involves scaling and polishing the remaining teeth, to clean them, keep them in good health for as long as possible, and avoid further tooth loss.
So, it’s safe to say that scaling and polishing are an important part of any dental procedure.
Dental scaling and polishing are often delegated to skilled veterinary technicians and nurses. So, when it comes time to invest in a new dental cleaning station, it’s a good idea for veterinarians and practice managers to review the equipment available and see what is required to meet their practice’s needs.
These common tools on a dental cleaning unit play a role in scaling and polishing:
Ultrasonic scaler. Hand scalers are still used, too, especially for tight spots that need extra attention. And curettes are needed for subgingival cleaning. However, it’s hard to beat an ultrasonic scaler for speed and efficiency when removing large amounts of dental calculus above the gumline. Many include a built-in LED light for easy visualization of the area being cleaned.
Polisher/Low-speed handpiece. This tool is crucial for smoothing over any small defects or microabrasions in the tooth enamel caused during scaling. In other words, polishing should ALWAYS follow scaling. Recent AAHA dental guidelines recommend using disposable prophy angles and individually packaged, fine-grit prophy paste with a polisher.
Air/Water syringe. This tool is useful for flushing away bits of tartar and other debris as you’re working, for drying a tooth prior to applying a sealant, or for irrigation and inspection of any visible subgingival areas after cleaning.
Suction tool. Weak suction can be a convenient way to remove excess water and saliva during a procedure.
Equipment for Drilling and Extractions
Many extractions require drilling into alveolar bone to expose the tooth root or divide the tooth into segments. This allows for safe and efficient extractions, with less risk of leaving root tips or fragments behind.
For this reason, a high-speed drill is an essential component of any veterinary dental cleaning station. The drill should have several burs to choose from, too, since veterinarians see patients of all different sizes and since different bur shapes (rounded or tapered, for example) serve different purposes.
In addition to the drill, hand tools—such as elevators, luxators, extraction forceps, and suture kits—will be used.
Other Factors to Consider In a Dental Cleaning Station
In addition to the tools available on the dental station, here are some considerations that may affect a veterinarian or practice owner’s decision to make a purchase…
The size of the unit. Practices with small spaces may prefer a compact cleaning station, while others might not have a size restriction.
Easy storage and access to tools. No matter the size of the station, it should be easy to store and access the tools right when you need to. No veterinary team member wants to fumble while reaching for a tool or accidentally drop something because it’s difficult to put back.
Water reservoirs. No one wants to run out of water (which is used for many of the tools, including drilling and ultrasonic scaling) during the middle of a procedure, then put things on hold as the reservoir is refilled. For that reason, it may be beneficial to look for a station with a larger distilled water reservoir capacity.
Service, maintenance, and warranty. It’s important to protect any equipment investment and to make sure it’s easy to keep the machine running so a veterinary practice can avoid canceling procedures due to equipment issues.
Also, remember to invest in high-quality complementary equipment. In addition to the dental cleaning station and other dental tools, a complete dental procedure also involves dental x-rays, appropriate anesthetic protocols and equipment, personal protection equipment, and anything else needed to perform a COHAT safely and effectively.
Veterinary dentistry can be a rewarding way to provide excellent patient care and generate income for a veterinary practice—a win-win scenario. To make sure these procedures run as smoothly as possible, it’s important to choose the equipment that’s the best fit for your practice’s needs.
Additional resources:
2019 AAHA Dental Care Guidelines for Dogs and Cats: https://www.aaha.org/globalassets/02-guidelines/dental/aaha_dental_guidelines.pdf
Editor’s Note:
Currently, we offer a complete veterinary dental cleaning station at an affordable price including shipping, delivery, and a 3-year warranty.
The space-saving machine is designed for high-volume use.
It features key tools that are crucial to any veterinary dental procedure—plus, a few exciting special features like advanced cooling for the high-speed drill, a scaler with an endodontics feature, an LED light on the polisher, and more!
Learn more, and contact us with any questions, here: https://newvetequipment.com/cleaning-station
Written by: Dr. Tammy Powell, DVM