Anesthesia & MRI: Minimizing Risk While Maximizing Image Quality
MRI is an imaging procedure, but a successful scan depends on much more than the machine.
Behind every good MRI study is a team carefully managing four important things:
Patient safety
Stable anesthesia
Efficient workflow
Clear, diagnostic images
For many veterinary teams, the anesthesia side of MRI can feel intimidating at first.
Not because it is impossible.
But because MRI is different.
The room is different.
The equipment is different.
The team setup is different.
And communication can feel different because the patient is not managed the same way as in a typical surgery room.
That is why preparation matters so much. When the team understands the MRI environment and has a clear plan before the scan begins, the entire process becomes safer, smoother, and more efficient.
Good MRI Images Start Before the Patient Enters the Scan Room
One of the easiest mistakes teams make early on is focusing only on the scan itself, but image quality starts long before imaging begins.
Things like:
Proper catheter placement
Organized line management
Patient padding
Stable anesthetic depth
Thoughtful positioning
…all directly impact the quality and efficiency of the study. A patient who’s uncomfortable, unstable, or poorly positioned often leads to:
Motion artifact
Repeat sequences
Longer anesthesia times
Increased stress for the entire team
Preparation matters more than people realize. And smooth MRI days usually come down to one thing: fewer preventable adjustments once the scan has started.
Positioning: Small Details Make a Huge Difference
Positioning is one of those things that can either save your team time or quietly steal a lot of it. Repeatable positioning helps create:
More consistent images
Faster sequence setup
Better study interpretation
Less need for rescans
Even small changes can matter, like:
Keeping the spine straight and supported
Avoiding rotation
Using consistent landmarks
Securing patients well enough to prevent subtle movement
The goal is stability without creating unnecessary pressure points or compromising ventilation. And from a workflow standpoint, consistency is everything.
When every technician positions slightly differently, studies become harder to reproduce and troubleshooting becomes more frustrating. That’s why many successful MRI teams eventually develop very standardized positioning protocols:
Same supports
Same setup sequence
Same communication process
It reduces guesswork for everyone involved.
Monitoring in MRI Environments Requires a Different Mindset
MRI anesthesia monitoring can feel uncomfortable at first because the setup naturally creates more distance between the patient and the anesthesia team.
You can’t always stand directly beside the patient the way you might during surgery. That’s why preparation and vigilance become even more important.
Some practical habits that help:
Confirm all monitoring equipment is MRI-compatible before the patient enters the room
Organize lines and cables carefully to prevent tangling or interference
Double-check connections before sequences begin
Establish clear communication between the imaging and anesthesia teams
And perhaps most importantly:
Anticipate problems early instead of reacting late
Because once imaging is underway, interruptions cost time, not just operationally, but anesthetically too.
Efficiency Between Sequences Matters More Than You Think
This is an area that often improves dramatically with experience. In the beginning, sequence transitions can feel slow:
Repositioning takes longer
Communication gets clunky
Adjustments happen reactively instead of proactively
But over time, efficient teams learn how to minimize downtime between sequences. That might look like:
Planning the study flow ahead of time
Anticipating coil changes early
Having positioning aids ready before they’re needed
Assigning clear responsibilities to each team member
The smoother those transitions become, the less time patients spend under anesthesia overall. And that benefits everyone:
Efficiency isn’t about rushing; it’s about reducing unnecessary delays.
Reducing Time Under Anesthesia Starts With Preparation
One of the best ways to shorten anesthesia time is surprisingly simple: be organized before induction ever happens. That includes:
Confirming imaging protocols ahead of time
Reviewing patient history thoroughly
Preparing supplies in advance
Ensuring the room is ready before bringing the patient in
Because once anesthesia begins, time matters. Even a few preventable delays can slowly compound:
Missing supplies
Positioning uncertainty
Communication breakdowns
Repeated setup adjustments
And those little inefficiencies add up quickly over the course of a full MRI day.
MRI Success Is Deeply Team-Dependent
One thing worth appreciating about MRI workflows is how clearly they highlight the importance of every role in the hospital. Successful MRI cases aren’t driven by one person. They rely on:
Veterinarians making thoughtful case selections
Technicians managing anesthesia and positioning
Assistants help maintain efficiency and patient safety
Imaging teams coordinating workflow and communication
When everyone understands the process, the entire experience becomes calmer and more controlled.
The Goal Isn’t Just Faster Scans
This is important. Efficiency matters, but not at the expense of patient care. The goal is not: “How fast can we get this done?”
The goal is: “How can we create consistent, high-quality studies while keeping patients as safe and stable as possible?”
When teams focus on preparation, communication, and repeatable workflow habits, both things tend to improve naturally:
Better image quality
Better anesthesia experiences
And over time, MRI shifts from feeling intimidating to feeling like just another well-coordinated part of patient care.
Common MRI Cases in General Practice (Not Just Specialty Hospitals)
When many people think about MRI in veterinary medicine, they picture massive specialty centers handling only the most advanced neurological cases.
But the reality is… a lot of the patients who benefit from MRI are already walking through the doors of general practices every single day. They’re the cases that leave you thinking:
“Something still isn’t adding up.”
“I feel like we’re missing a piece of the puzzle.”
“We’ve tried conservative management, but we still don’t have answers.”
And honestly, that’s where MRI becomes so valuable.
Not because every patient needs advanced imaging, but because some cases simply can’t be fully understood without it.
The interesting part? These aren’t always rare or highly specialized cases. Many of the patients you’re already seeing regularly, you just don’t always have the diagnostic clarity to confidently move forward.
The Suspected IVDD Case
This is probably one of the most recognizable MRI cases in veterinary medicine.
The painful dachshund.
The suddenly non-ambulatory Frenchie.
The patient went from “a little stiff” to neurologic symptoms seemingly overnight.
In many cases, you can strongly suspect IVDD based on exam findings and history alone. But MRI helps answer the deeper questions:
Which disc is affected?
How severe is the compression?
Is surgery indicated?
Are there multiple sites involved?
That level of detail matters—not only for surgical planning, but for setting realistic expectations with clients.
And sometimes, MRI reveals something entirely different than what was initially suspected.
That’s the part that turns educated guesses into confident treatment plans.
The Seizure Workup That Needs More Than Monitoring
Seizure cases can be incredibly frustrating for both veterinarians and pet owners.
Sometimes, everything points toward idiopathic epilepsy. Other times… something feels off.
Maybe:
The patient is older at onset
Neurologic deficits are present between episodes
Medications aren’t helping the way you expected
Episodes are becoming more frequent or severe
MRI becomes especially valuable in these situations because it helps determine whether there’s an underlying structural cause:
Brain tumors
Inflammatory disease
Congenital abnormalities
Previous trauma or infarcts
And for clients, having clearer answers often improves their ability to commit emotionally and financially to treatment plans. Even when findings are difficult, clarity helps families make more informed decisions moving forward.
Chronic Lameness Cases That Keep Circling Back
Every practice has them…the patient that’s had:
Multiple radiographs
Rest periods
Medication trials
Rehab recommendations
…but still isn’t improving the way everyone hoped.
Sometimes the issue isn’t orthopedic at all. MRI can uncover:
Soft tissue injuries
Neurologic involvement
Subtle joint abnormalities
Muscle or tendon pathology that radiographs simply can’t show well
And these are often among the most diagnostically rewarding cases because the answer has been hiding in plain sight all along.
It’s not that the case was being managed incorrectly—it’s that the full picture wasn’t visible yet.
The “Painful but Normal Diagnostics” Patient
These cases can be some of the most mentally exhausting.
The patient is clearly uncomfortable. The owner knows something is wrong. Your team knows something is wrong, but bloodwork looks normal, radiographs are inconclusive, and conservative management only partially helps.
These are the moments where MRI can completely shift the direction of a case. Whether it’s:
Spinal cord compression
Nerve root involvement
Inflammatory disease
Hidden soft tissue pathology
…advanced imaging often provides the missing explanation everyone has been searching for. And perhaps just as importantly, it gives clients reassurance that their concerns were valid all along.
MRI Isn’t About Replacing Clinical Skills
This is important: MRI doesn’t replace a strong physical exam, thoughtful diagnostics, or clinical intuition.
If anything, it enhances them.
Because most MRI cases don’t begin with imaging. They begin with experienced veterinary teams recognizing:
“This patient needs more answers than we can get from our current diagnostics.”
That’s good medicine, not overcomplication.
General Practice Is Already Seeing MRI Cases
This is where the conversation around MRI has really started to shift in recent years. Advanced imaging is no longer reserved exclusively for referral hospitals handling ultra-rare cases.
General practices are already seeing:
Neurologic patients
Chronic pain cases
Complicated lameness workups
Patients that plateau despite treatment
The difference is that now, more practices are exploring ways to keep those diagnostic journeys closer to home. And for many hospitals, that changes:
Continuity of care
Client trust
Diagnostic confidence
Long-term case management
Sometimes the Biggest Value Is Simply Having Answers
At the end of the day, MRI isn’t just about finding dramatic diagnoses.
Sometimes, its greatest value is ruling things out or confirming a suspicion.
Sometimes it’s helping a client finally understand why their pet hasn’t improved.
And sometimes, it simply allows everyone, the veterinarian, the team, and the owner, to stop operating in uncertainty.
Because you’re already seeing these cases. You just don’t always have all the answers yet.
90 Free Facebook Post Prompts
Free ebook
90 Free Facebook Post Prompts for Veterinary Clinics
Many veterinary clinics want to post more often on Facebook.
But the hard part is knowing what to say.
That blank screen can slow everything down.
This free ebook solves that problem.
It gives veterinary clinics 90 ready-to-use Facebook post prompts that can be copied, customized, scheduled, and reused.
What is inside the ebook?
The ebook includes a simple system for creating Facebook posts with AI.
Inside, you get:
A reusable master prompt
90 veterinary Facebook post ideas
A simple posting system
Tips for scheduling and recycling content
Practical reminders about reviewing AI posts before publishing
The goal is simple: help your clinic stay visible without making social media feel like a daily chore.
What kind of posts can you create?
The prompts cover real veterinary topics that pet owners care about.
Topics include:
Puppy care
Kitten care
Wellness exams
Vaccines
Dental care
Parasite prevention
Senior pet care
Surgery prep
Heatstroke prevention
Toxic foods
Urgent care reminders
Lost pet safety
Team appreciation
These are helpful, practical topics that keep your clinic visible and useful in a pet owner’s Facebook feed.
Why image posts work well
Facebook posts do not need to be complicated.
A strong image post can quickly convey a single helpful idea.
The best posts are often:
Short
Friendly
Easy to scan
Visually clear
Focused on one topic
Helpful to pet owners
A simple checklist can work very well.
For example:
Watch for warning signs
Call your vet when needed
Keep preventive care current
That kind of content is easy for pet owners to understand and remember.
AI can help you move faster, and your clinic should always review the final post.
Before publishing, check:
Medical accuracy
Clinic voice
Spelling
Logo placement
Phone number
Address
Any wording that could sound like individual medical advice
Let AI help with speed. Let your clinic protect quality.
Your clinic does not need to reinvent Facebook every week.
Start with good prompts.
Create useful posts.
Schedule them.
Recycle the best ones.
Keep showing up.
That is how your clinic can stay visible without adding more stress to an already busy week.
Click here to download the free ebook and get 90 free Facebook post prompts your veterinary clinic can start using today.
The 90-Post Facebook System
How to Build a Simple 90-Post Facebook System for Your Veterinary Clinic
Posting on Facebook does not have to feel random.
It does not have to be rushed.
It does not have to depend on someone “remembering” to post.
With the right system, your clinic can stay visible without having to start from scratch every day.
The simple math
Here is an easy system:
3 posts per day
5 days per week
15 posts per week
6 weeks = 90 posts
That gives your clinic a full library of useful Facebook content.
That is not random posting.
That is a real content system.
Why this works
Most veterinary topics are evergreen.
That means they stay useful over time.
Examples include:
Wellness exams
Vaccines
Parasite prevention
Dental disease
Heat safety
Microchips
Toxic foods
Senior pet care
Surgery prep
Lost pet reminders
These topics do not expire after one post.
You can reuse them later with a new image, headline, caption, or seasonal angle.
That is not lazy. That is smart.
The content loop
Once you create your 90 posts, number them.
Post #1.
Post #2.
Post #3.
And so on.
Then schedule them in Facebook’s scheduler.
When you reach post #90, start again with post #1.
You can update, refresh, or improve posts as needed.
What AI does
AI helps create the content.
It can help you:
Create the first draft
Turn one topic into several versions
Keep the wording simple
Create short checklists
Make posts more scan-friendly
Save time
What your clinic does
Your clinic still approves the final post.
Before publishing, ask:
Is this accurate?
Is it easy to understand?
Is it friendly and helpful?
Does it sound like our clinic?
Did we avoid individual medical advice?
Is the spelling correct?
Is the phone number correct?
Is the logo correct?
AI helps create. Your clinic protects trust.
The bottom line is consistency works.
When pet owners see helpful posts from your clinic again and again, your clinic stays top of mind.
You do not need a complicated marketing plan.
You need a simple content library, a schedule, and a repeatable process.
Want the full system? Click here to download the free ebook with 90 ready-to-use Facebook post prompts for veterinary clinics.
AI Helps Veterinary Clinics Stay Visible
How AI Helps Veterinary Clinics Stay Visible on Facebook
Most veterinary clinics know they should post on Facebook more often.
But in the real world, social media often gets pushed aside.
Appointments come first.
Surgeries come first.
Phone calls come first.
Emergencies come first.
The problem is not that your clinic has nothing to say.
The problem is finding the time to say it.
That is where AI can help.
The big idea
AI can help your clinic create Facebook posts faster, easier, and more consistently.
It can help you:
Brainstorm post ideas
Write captions
Turn one topic into several posts
Simplify pet care topics
Avoid starting from a blank screen
Stay active without spending hours every week
The goal is not to replace your team.
The goal is to give your team a faster starting point.
Why Facebook still matters
Many pet owners may not visit your website every week.
But they do scroll Facebook.
That gives your clinic a simple way to stay visible between appointments.
Helpful Facebook posts can remind pet owners about:
Wellness exams
Vaccines
Parasite prevention
Dental care
Senior pet needs
Seasonal safety
When to call the vet
Visibility builds familiarity.
Familiarity builds trust.
Trust helps pet owners think of your clinic first.
Keep it simple
A good Facebook post does not need to be long.
It needs to be:
Clear
Friendly
Useful
Easy to read
Accurate
Consistent with your clinic’s voice
Pet owners are busy. They do not need a lecture.
They need quick, helpful reminders that make pet care easier.
AI is a tool, not a veterinarian
AI should help with writing, organizing, and creating first drafts.
It should not diagnose a pet.
It should not give individual medical advice.
It should not replace your clinic’s judgment.
Best rule: Let AI create the first draft. Let your clinic approve the final version.
Before anything goes live, review it carefully.
Check the facts.
Check the tone.
Check the spelling.
Check the clinic name, phone number, address, and logo.
Small mistakes matter online.
The bottom line
Your clinic does not need to become a media company.
You just need a simple way to stay visible, helpful, and consistent.
AI can make Facebook posting easier.
A good prompt can make it faster.
A repeatable system can make it something your clinic actually maintains.
Want the easy way to start? Click here to download the free ebook with 90 ready-to-use Facebook post prompts for veterinary clinics.
From Referral to Diagnosis: The MRI Patient Journey in a Busy Practice
When practices first start considering MRI, it’s easy to focus on the machine itself.
The specs. The installation. The financial investment.
But eventually another question surfaces: “What would this actually look like in our hospital day-to-day?”
And honestly, it’s such a good question to ask.
Because successful MRI integration isn’t just about having advanced imaging, it’s about creating a workflow that feels manageable, efficient, and sustainable for your team.
The good news is that most practices don’t build perfect MRI workflows overnight. They build them one protocol, one patient, and one team adjustment at a time.
Let’s walk through what the MRI patient journey can realistically look like inside a busy veterinary practice.
It Starts Before the Appointment Is Even Scheduled
One of the biggest shifts in practice experience after adding MRI is becoming more intentional about case selection. Not every patient needs advanced imaging. But the right cases become much clearer over time.
Common MRI candidates often include:
Suspected IVDD cases
Seizure patients
Chronic neurologic symptoms
Unexplained pain or lameness
Patients are not responding to treatment as expected
As your team gains confidence, scheduling becomes more streamlined because everyone begins to recognize which cases are most likely to benefit from MRI. That’s where strong communication between doctors, technicians, and client care teams becomes incredibly important.
When everyone understands which patients are appropriate candidates, which diagnostics should be performed beforehand, and how to prepare clients for the process, the entire workflow runs more smoothly before the patient even walks through the door.
The Day-of Workflow: Organized, Not Chaotic
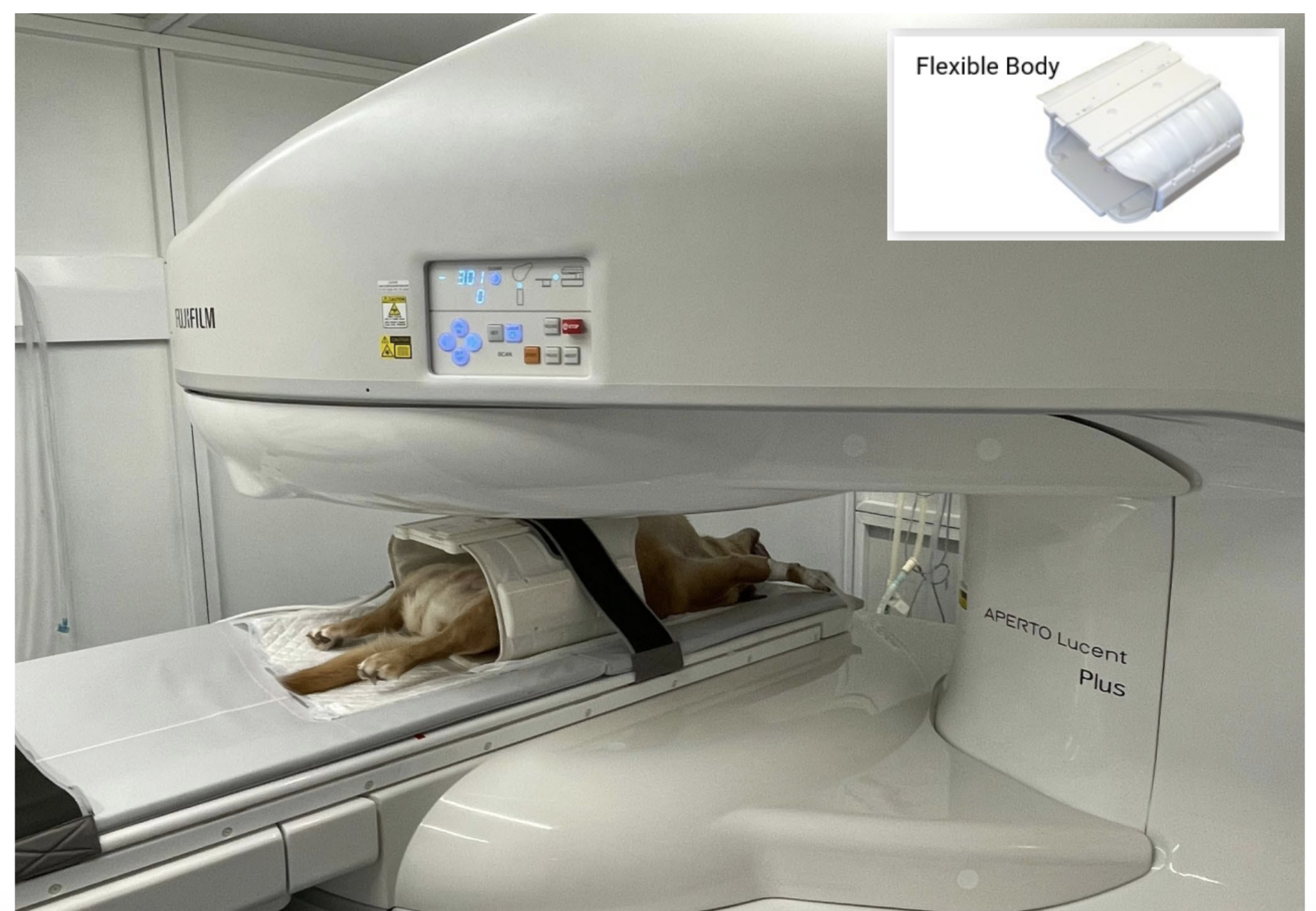
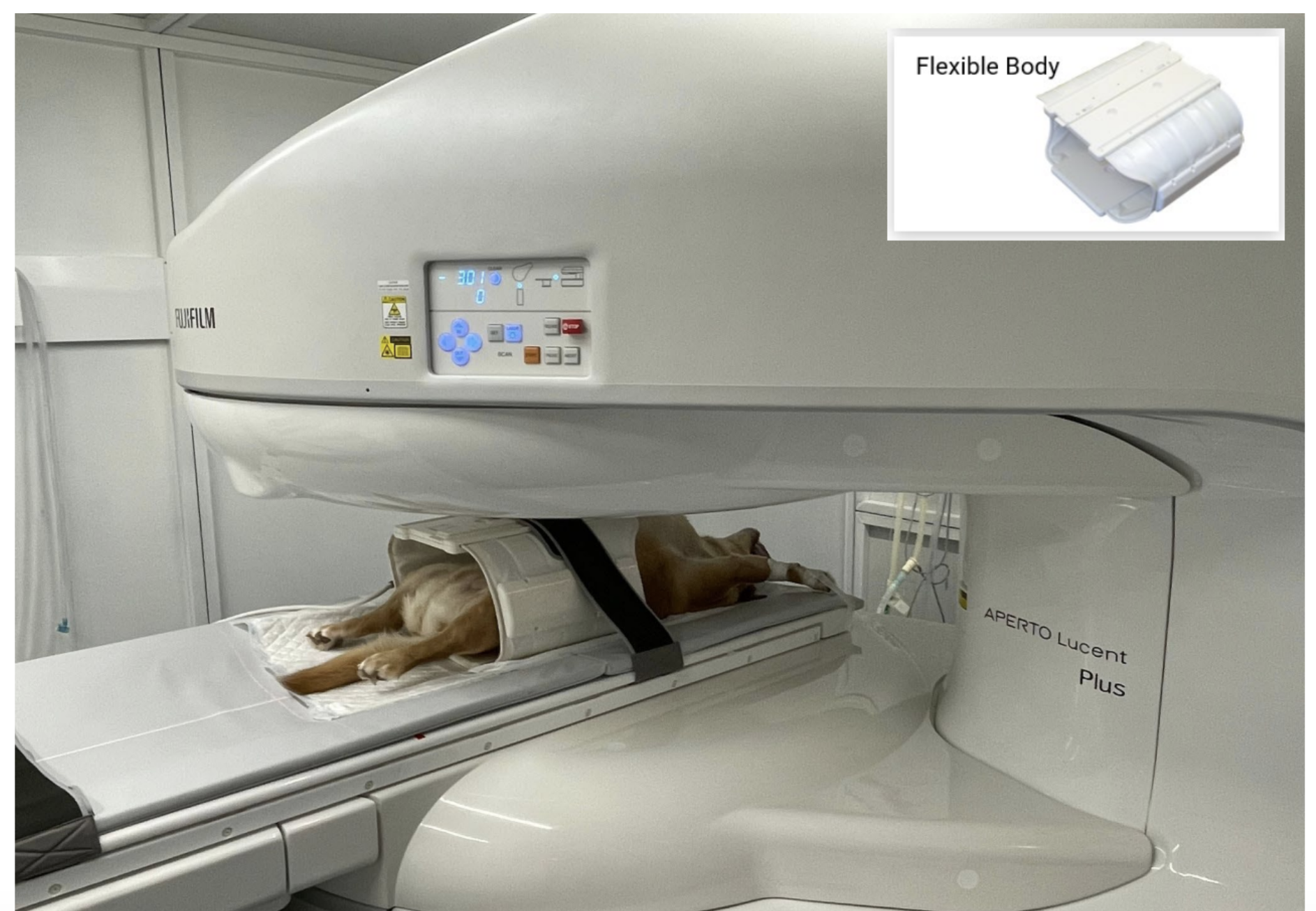
From the outside, an MRI can seem an intimidating operation. In reality, many practices discover that once protocols are established, MRI days become surprisingly structured. Especially using an MRI like theFujifilm Aperto Lucent 0.4T MRI system.
Typically, the workflow looks something like this:
Morning admission and patient assessment
Sedation or anesthesia preparation
MRI safety checks
Positioning and imaging
Recovery and monitoring
Image review and reporting
The key is consistency. The more repeatable your protocols become, the less stressful the process feels for everyone involved. And unlike many areas of veterinary medicine, which can feel unpredictable by nature, MRI often rewards preparation and routine.
Team Roles Matter
MRI is one of the clearest examples of how veterinary medicine truly functions as a team effort. A smooth imaging day depends on multiple moving pieces working together:
Veterinarians selecting appropriate cases
Technicians managing anesthesia and positioning
Assistants supporting patient handling and workflow
Client care teams coordinating communication and scheduling
Every role impacts efficiency. And interestingly, many hospitals find MRI creates opportunities for team growth:
Technicians developing advanced anesthesia skills
Staff are becoming more confident with neurology cases
Improved collaboration between departments
For some teams, adding MRI becomes more than a service expansion—it becomes a professional development opportunity across the hospital.
Positioning and Preparation Can Make or Break the Scan
One thing that practitioners learn quickly is that MRI quality doesn’t depend solely on the machine itself. Patient preparation matters. Good positioning:
Improves image consistency
Reduces repeat sequences
Shortens anesthesia time
Helps radiologists interpret studies more accurately
And in busy hospitals, efficiency matters. Even small improvements in preparation and workflow can significantly reduce recovery times, improve scheduling, and lower stress levels.
That’s why many successful MRI programs focus heavily on protocol refinement early on.
Report Turnaround: Where Answers Start Taking Shape
For both clients and clinicians, the moment that matters most… when the scan is complete. Now everyone wants answers. Depending on the hospital setup, MRI studies may be:
Reviewed internally by specialists
Sent to teleradiology services
Interpreted collaboratively between teams
Fast, clear reporting can dramatically improve workflow momentum:
Treatment plans move forward faster
Surgical decisions happen sooner
Client communication becomes more confident and direct
And perhaps most importantly, patients spend less time in diagnostic limbo. That’s something both veterinary teams and pet owners deeply appreciate.
The Reality: Workflow Evolves Over Time
No MRI workflow is perfect from day one. There will be adjustments:
Scheduling tweaks
Protocol refinements
Team training moments
Efficiency improvements
That’s normal. The practices that succeed with MRI aren’t necessarily the ones that start with flawless systems; they’re the ones willing to continuously refine the process as their confidence grows.
And over time, what once felt like a major operational leap simply becomes another integrated part of how the hospital delivers care.
MRI ROI Calculator
Total Cases to Pay Off: 0
Weekly Revenue: $0
Monthly Revenue: $0
Yearly Revenue: $0
Time to Pay Off Machine:
0 Years
How MRI Improves Client Trust and Case Acceptance
One of the hardest parts of veterinary medicine isn’t always making the diagnosis.
Sometimes, it’s helping clients feel confident enough to move forward with the next step.
You can have the right instincts, the right experience, the right treatment plan, but when a client is scared, overwhelmed, or struggling to fully understand what’s happening with their pet, hesitation naturally follows.
That’s where MRI can change the conversation in a powerful way.
Not because it’s flashy technology or advanced imaging…
But because it brings something clients desperately want during stressful moments: Clarity.
When “We Think” Becomes “We Know”
There’s a big emotional difference between: “We suspect there may be a spinal issue…”
and “Here’s exactly what we’re seeing.”
MRI gives clients something tangible. Instead of trying to visualize a problem through explanations alone, they can often see that something is wrong.
That clarity changes the tone of the conversation almost immediately. Suddenly:
Recommendations feel more concrete
Treatment plans feel more justified
Decisions feel less uncertain
And for many clients, that makes moving forward feel far less intimidating.
Confidence Builds Trust
Clients don’t expect veterinarians to have all the answers instantly. What they’re looking for is confidence that their pet is being guided thoughtfully and thoroughly.
Advanced imaging reinforces that trust.
When you’re able to pursue deeper diagnostics in-house, clients often perceive:
A higher level of medical capability
Greater continuity of care
A more proactive approach to their pet’s health
That doesn’t mean every case needs an MRI - far from it. But when MRI is recommended, it says, “We’re committed to finding answers, not just managing uncertainty.”
MRI Helps Clients Understand the “Why”
One of the biggest barriers to case acceptance isn’t always cost; often, it’s confusion. If clients don’t fully understand why additional diagnostics are needed, what information MRI provides, or how results impact treatment decisions, it becomes much harder for them to say yes.
MRI creates opportunities for clearer education:
Showing a compressed spinal cord
Identifying a brain lesion
Explaining why surgery is, or isn’t, the best option
Those visual conversations are often far more impactful than words alone.
For many clients, seeing the problem helps them emotionally process the seriousness of the situation in a way that verbal explanations sometimes can’t.
Keeping Care Within One Trusted Team
There’s another layer to client trust that often gets overlooked: continuity.
When patients are referred elsewhere for imaging, clients suddenly find themselves:
Retelling their story
Meeting a new medical team
Navigating an unfamiliar hospital
Waiting for communication between providers
Even when referral relationships are excellent, the experience can still feel fragmented from the client’s perspective. Offering MRI within your own hospital can create a much more connected experience:
Familiar faces
Consistent communication
One team guiding the case from start to finish
That continuity builds reassurance during what’s often a stressful and emotional time.
Better Understanding Often Leads to Better Compliance
When clients clearly understand a diagnosis, they’re more likely to follow through with treatment recommendations. That can mean:
Moving forward with surgery sooner
Committing to rehabilitation plans
Understanding realistic prognoses
Staying engaged in long-term management
MRI doesn’t just influence the initial decision; it can improve compliance throughout the entire treatment journey. And ultimately, better compliance often leads to better patient outcomes.
The Emotional Value of Answers
Anyone who’s worked in veterinary medicine long enough has seen it:
Sometimes the hardest part for clients is not knowing.
The uncertainty. The waiting. The fear of making the wrong choice.
MRI can’t fix every diagnosis. It can’t guarantee every outcome, but it can provide direction.
And even when the news isn’t ideal, many clients feel relief simply having clearer answers and a defined plan moving forward.
That emotional value is easy to underestimate, but incredibly important.
Technology Matters. Communication Matters More.
At the end of the day, MRI itself doesn’t create trust; people do.
The technology supports stronger conversations:
More confident recommendations
Better client education
Clearer expectations
More informed decision-making
When used thoughtfully, MRI becomes more than an imaging tool. It becomes a bridge between medical knowledge and client understanding.
And in a profession built on relationships, that connection matters just as much as the images themselves.
Choosing the Right Veterinary MRI: A Practical Guide for Real-World Decision Making
If you read thelast article and found yourself thinking, “Okay… MRI might actually make sense for us,” the next question is usually where things get a little murky:
“Which system do we even choose?”
This is where many practices get stuck: there’s so much information, and not all of it feels relevant to your day-to-day.
So instead of diving into spec sheets and technical jargon, let’s simplify this.
There are three key players you’ll see again and again in the veterinary MRI space:Fujifilm, Esaote, and Hallmarq Veterinary Imaging.
Each brings something different to the table, and the “right” choice has a lot less to do with which system is best and a lot more to do with which system fits your practice.
Let’s walk through the differences in a way that actually helps you decide.
1. Workflow: How Will This Fit Into Your Day?
This is one of the most overlooked (and most important) factors.
Some MRI systems are built for high-volume, fast-paced environments where efficiency is everything. Others are designed with simplicity and accessibility in mind.
Systems from Hallmarq Veterinary Imaging are often praised for their workflow-friendly design. They’re designed specifically for veterinary use, which shows up in intuitive interfaces and streamlined protocols.
Esaote systems also lean into ease of use, especially with low-field MRI. Many practices appreciate the shorter learning curve and smoother integration into general practice workflows.
Fujifilm tends to bring a more advanced imaging environment, often with greater customization and capability.
2. Footprint & Installation: What Does This Actually Look Like in Your Hospital?
MRI isn’t just a piece of equipment; it’s an infrastructure decision.
This is where real-world constraints come into play:
Available square footage
Structural considerations
Power requirements
Shielding and site prep
Esaote is known for its compact systems, which are a good fit for general practices or smaller specialty hospitals.
Hallmarq Veterinary Imaging also offers purpose-built veterinary systems, often designed to fit into existing clinical spaces compared to traditional human MRI units.
Fujifilm Healthcare systems are known for their robust infrastructure and high performance.
Before you fall in love with any system, make sure it realistically fits your space, your buildout timeline, and your tolerance for construction.
3. Image Quality vs. Throughput: What Do You Actually Need?
This is where conversations can get… a little heated. High-field vs. low-field. Resolution vs. speed. Detail vs. practicality. Here’s the grounded version:
Fujifilm Healthcare systems are often associated with higher field strengths and advanced imaging capabilities, which can deliver exceptional detail—especially valuable for complex neurological cases.
Esaote focuses heavily on low-field MRI, which is more than capable for many common veterinary applications.
Hallmarq Veterinary Imaging offers systems designed to balance usefulness with practical workflow, particularly in veterinary-specific applications.
But here’s the key question to ask:
Are you optimizing for the most advanced image possible, or the most usable system for your caseload?
Because those aren’t always the same thing.
4. Service & Support: What Happens After Installation?
This is the part no one gets excited about, until something goes wrong.
MRI uptime matters. Delays cost money, disrupt schedules, and create stress for your team.
Hallmarq Veterinary Imaging has a sound reputation for its support and repair services.
Esaote provides accessible support and training, particularly helpful for practices newer to MRI.
Fujifilm Healthcare benefits from the backing of a large, global imaging company, which can translate into robust service networks and advanced technical resources.
The takeaway: Don’t just ask if service is available, ask:
How fast is the response time?
What does training look like?
Who do we call when something feels “off”?
So… How Do You Choose?
At the end of the day, this isn’t about picking the “best” MRI system.
It’s about choosing the one that aligns with:
Your caseload
Your team’s experience
Your physical space
Your growth goals
A system that looks incredible on paper but slows down your workflow or overwhelms your team isn’t a win. On the flip side, a system that fits seamlessly into your day, even if it’s not the most “advanced” option available, can completely transform how you practice.
Is MRI Worth It for Your Practice? A Real-World Discussion
If you’ve ever found yourself sending a case out for advanced imaging and thinking,
“I wish we could keep this in-house.”
You’re not alone.
For many veterinary practices, MRI sits in that category of “maybe someday.” It feels like a big leap, financially, operationally, and even mentally. But the conversation around MRI has shifted more recently. It’s no longer just for large specialty centers. More general and hybrid practices are starting to ask a very practical question:
Does this actually make sense for my hospital?
Let’s break that down in a way that feels real.
It’s Not Just the Cost, It’s the Cases You’re Losing
When most practices evaluate MRI, the first number they look at is the price tag. That’s fair. But focusing only on upfront cost can miss the bigger picture.
Think about the cases you’re already seeing:
The down dog with suspected IVDD
The seizure workup that needs answers
The chronic lameness case that just isn’t adding up
Right now, what happens to those patients?
They get referred out.
And when they leave, a few things often go with them:
Diagnostic revenue
Treatment plans
Follow-up care
Long-term client loyalty
Not every referral is lost forever, but many don’t come back in the same way. MRI changes that dynamic. It allows you to keep the case, guide the course of care, and remain at the center of the patient’s care.
Revenue Per Scan Adds Up Faster Than You Think
Let’s keep this easy.
MRI isn’t about running dozens of scans a day. In fact, many successful veterinary practices start with just a handful of cases per week. Even at a conservative pace:
A few scans per week
Consistent demand from neurology and complex cases
Gradual growth as your team gains confidence
That can translate into meaningful, steady revenue, not just from the scan itself, but from everything that follows:
Surgical procedures
Ongoing treatment plans
Rechecks and monitoring
MRI often feeds into the rest of your services.
Referral Retention vs. Referral Dependence
There’s nothing wrong with referring. In many cases, it’s absolutely the right call.
But there’s a difference between strategic referral and default referral.
When MRI isn’t available in-house, even cases you could manage often get sent elsewhere simply because you don’t have the diagnostic clarity to move forward confidently.
Bringing MRI into your practice shifts that balance and you refer when it truly benefits the patient, not just when you’re missing a diagnostic piece
That distinction matters for both patient care and business sustainability.
The Confidence Factor (For You and Your Clients)
There’s also a less tangible, but incredibly important, ROI: confidence.
When you can move from “this is what we think is going on…” to “this is what we’re seeing and here’s the plan…”
…it changes everything.
Clients feel it, and decision-making becomes clearer and faster.
That level of clarity often leads to:
Higher case acceptance
Stronger trust
Better compliance with treatment plans
MRI provides answers, and we all know how powerful clear answers can be.
Growth Doesn’t Have to Mean Overwhelm
One of the biggest hesitations around MRI is the fear of disruption:
Will this slow us down?
Can our team handle it?
Is this going to complicate our workflow?
Those are certainly valid concerns, but they’re also manageable. Many practices gradually integrate MRI, starting with select case types, building protocols over time, and training the team in phases.
It doesn’t have to be an overnight transformation. In fact, the most successful implementations rarely are.
So… Is It Worth It?
The honest answer is: it depends on your goals. But if your practice is:
Seeing a steady stream of complex cases
Looking to retain more advanced diagnostics
Wanting greater control over patient outcomes
Focused on long-term growth rather than short-term volume
…then MRI becomes less of a “nice to have” and more of a strategic next step.
MRI ROI Calculator
Total Cases to Pay Off: 0
Weekly Revenue: $0
Monthly Revenue: $0
Yearly Revenue: $0
Time to Pay Off Machine:
0 Years
Built for Busy Surgery Days: Making the Most of the Veta 3X in High-Volume Veterinary Practices
In a practice where surgery days stack up quickly, and anesthesia is part of the daily rhythm, your equipment has to do more than just function. It needs to keep up with the pace.
When you’re moving from one procedure to the next, efficiency, consistency, and ease of use start to matter just as much as performance.
That’s where a system like the VETA 3X really supports a high-volume environment, especially when it’s set up and used intentionally.
Keeping Turnover Smooth Between Cases
In busy hospitals, the time between procedures can add up fast. Small inefficiencies like switching circuits, adjusting setups, or troubleshooting equipment can slow your entire day.
The VETA 3X has both rebreathing and non-rebreathing options readily available (including the Bain system setup), allowing for quicker transitions between patients of different sizes. Instead of reworking your setup each time, your team can move efficiently from one case to the next.
Tip: Keep commonly used circuits (like your Bain and standard rebreathing system) prepped and easily accessible. Even shaving a few minutes off each case can significantly improve overall flow.
Supporting Consistency Across Multiple Team Members
In high-volume settings, anesthesia isn’t managed by a single person; it’s often shared among technicians and doctors throughout the day. That makes equipment consistency especially important.
The VETA 3X layout and accessible controls help create a more consistent experience for everyone who uses it. When each team member knows exactly where to look and what to expect, it reduces variability in setup and monitoring.
Consideration: Standardize your anesthesia protocols alongside your equipment. When your machine and your processes align, it creates a smoother, safer experience across the board.
Reducing Setup Fatigue
On long surgery days, even experienced teams can feel the effects of repetition. Equipment that’s overly complex or difficult to handle increases the risk of small errors, especially later in the day.
A streamlined system with clearly organized components helps reduce that mental load. Features like the fixed-mount pour-fill vaporizer and simple hose connections mean fewer steps and less second-guessing during setup.
Tip: Build a quick pre-anesthesia checklist specific to your machine. This helps catch small issues early and keeps your team consistent, even during busy or fatiguing days.
Managing Smaller Patients Efficiently
High-volume practices often see a mix of routine procedures: spays, neuters, dentals, many involving smaller patients. Having a reliable non-rebreathing option readily available is essential.
The included Bain system kit and disposable Bain circuit make it easier to quickly set up for these cases without needing additional equipment or adjustments.
Consideration: Keep a dedicated small-patient anesthesia station or a similar setup if your caseload leans heavily in that direction. It minimizes switching and keeps your workflow tighter.
Planning for Maintenance Without Disruption
In a busy practice like yours, downtime isn’t just inconvenient; it can throw off your entire schedule. Reliable equipment helps, but proactive maintenance matters just as much.
The VETA 3X's simple design and accessible components make routine checks and maintenance more manageable, which is key when you’re relying on it daily.
Tip: Schedule brief, regular equipment checks (daily quick checks, weekly deeper reviews) rather than waiting for issues to arise. It’s far easier to prevent disruptions than to work around them mid-day. (see tips below)
The Bigger Picture
Your day already demands a lot: balancing a packed surgical schedule, managing your team, handling administrative responsibilities, and navigating the emotional weight of patient care.
The last thing you need is equipment that adds friction or uncertainty.
Your anesthesia machine should be one of the most dependable parts of your workflow, something your team can trust without hesitation. When that piece is solid, it’s one less thing pulling your attention, and one more way to support a smoother, more manageable day.
Daily Quick Checks (The "Pre-Flight" Routine)
Perform these every morning before the first patient is prepped.
Perform a High-Pressure Leak Test: Close the pop-off valve, occlude the Y-piece (with your thumb or a stopper), and use the $O_2$ flush to pressurize the system to 30 cmH2O. Ensure the pressure holds for at least 10–15 seconds.
Check Vaporizer Levels: Ensure the vaporizer is filled to the appropriate line. Verify the fill cap is tightened securely to prevent anesthetic gas leaks.
Inspect CO2 Absorbent: Check the color of the soda lime or Baralyme. If 1/3 to 1/2 of the canister has changed color (usually to purple), replace it immediately. Remember: color can "revert" overnight, so trust your usage logs if the granules look white but are exhausted.
Oxygen Supply Verification: Check your tank pressure or central line. Ensure you have more than enough volume to get through the day's scheduled procedures.
Verify Scavenging Connection: Ensure the scavenging interface (active or passive) is properly connected, and the charcoal canister (if used) is not expired by weight.
The "Open Pop-Off" Rule: Immediately after your leak test, re-open the pop-off valve. A closed pop-off valve is a leading cause of barotrauma.
Weekly Deeper Reviews
Schedule these for a specific day (e.g., Friday afternoon) to prep for the coming week.
1. Seal and O-Ring Inspection
Check the O-rings on the vaporizer mounting and the CO2 canister. Dry or cracked O-rings are the primary source of "phantom leaks" that are hard to find during daily checks.
Apply a tiny amount of medical-grade lubricant if seals appear dry.
2. Breathing Circuit & Bag Integrity
Fully extend your breathing hoses and check for small cracks or "milky" discoloration in the plastic.
Inflate your reservoir bags and check for brittleness or tiny pinholes, especially around the neck where they connect to the machine.
3. One-Way Valve (Flutter Valve) Inspection
Unscrew the clear domes over the inspiratory and expiratory valves.
Ensure the thin discs are clean, dry, and not "sticking" due to moisture or residue. A sticking valve can cause a patient to re-breathe $CO_2$.
4. Flowmeter Function
Turn the oxygen flowmeter up and down slowly. Ensure the bobbin or ball moves smoothly without sticking or "jumping," which can indicate debris in the flow tube.
5. Bain System / Non-Rebreathing Kit
Since the Veta 3X is often used for smaller patients, inspect the inner tube of the Bain circuit. Ensure it is not disconnected or kinked, as this can lead to a failure in delivering fresh gas to the patient.
5 Factors That Make or Break Your Next Veterinary Anesthesia Machine Purchase
Investing in a new anesthesia machine is one of those decisions that quietly shapes your entire surgical workflow. It’s so important to choose equipment your team can rely on every single day, across every patient, in every procedure.
If you’re in the process of evaluating options, here are five key factors worth paying close attention to.
Let’s dive in…
1. Reliability of Anesthetic Delivery
At the core of any anesthesia machine is its ability to deliver consistent, controlled anesthesia. Variability can directly impact patient stability, so, as you know, it’s not something to be taken lightly.
Look for systems with dependable vaporizers and pressure management features that help maintain steady anesthetic depth throughout a procedure.
A fixed-mount isoflurane vaporizer with a pour-fill system, like the one included with the Veta 3X, supports consistent output while minimizing handling complexity.
This is one area where simplicity and precision go a long way.
2. Compatibility with Your Patient Base
Not every practice has the same caseload, and your anesthesia machine should reflect that.
If you’re seeing a wide range of patients, from small cats and exotics to larger dogs, you’ll want flexibility in your breathing systems.
Machines that support both rebreathing and non-rebreathing setups allow you to adapt quickly without needing separate equipment. The inclusion of a Bain system kit and disposable Bain circuit makes it easier to safely anesthetize smaller patients without overcomplicating your setup.
Versatility here directly translates to smoother case flow.
3. Ease of Use for Your Team
Anesthesia is managed by a team, often in fast-paced environments. Intuitive, easy-to-use equipment reduces training time and helps minimize errors.
Features to look for:
Clearly labeled and accessible controls
Logical component layout
Straightforward switching between systems
When components like the APL valve, CO₂ absorber, and breathing circuits are easy to access and manage, your team can stay focused where it matters most…on the patient.
It’s also worth considering how well a new anesthesia machine will integrate into your existing workflow without slowing your team down.
The goal is to create a smoother, more predictable surgical environment. Equipment that’s quick to set up, easy to maintain, and intuitive to use can reduce delays between cases and help your team stay efficient throughout the day.
4. Included Components and Setup Readiness
One of the most overlooked factors when purchasing a new anesthesia machine is what actually comes with it. A more complete system, like one that includes:
Fixed mount Iso vaporizer (pour fill)
O₂ hose
US gas hoses (DISS/DISS)
Bain system kit
Disposable Bain circuit
…allows your team to get up and running quickly without sourcing additional parts or troubleshooting compatibility issues.
It’s a small detail that makes a big difference during setup.
5. Cost, Warranty, and Long-Term Value
Price always matters, but it should be evaluated alongside what you’re actually getting.
A system priced at $4,000 (including shipping) with a 3-year parts-only warranty offers a clear, predictable investment. Beyond the upfront cost, consider:
Expected lifespan of the equipment
Ease of maintenance
Availability of replacement parts
A well-balanced machine provides not just affordability, but dependable performance over time, without constant repairs or workarounds.
Reliability Where It Counts
Choosing the right anesthesia machine goes beyond specs on a page. It’s about finding a system that fits your patients, supports your team, and performs consistently under real clinical conditions.
When you evaluate options through that lens, reliability, flexibility, usability, completeness, and long-term value, you’re far more likely to land on a machine that truly supports your practice day in and day out.
The Mindray Veta 3X: Reliable Anesthesia for Modern Veterinary Practices
As an experienced pro in veterinary surgery, you know that your anesthesia machine is a critical component of maintaining safe, controlled procedures.
When equipment is reliable, intuitive, and easy to integrate into the workflow, it supports patient safety and team efficiency.
That’s where the Mindray Veta 3X Anesthesia Machine fits in.
Before we dive into the details, let’s revisit the importance of choosing the right anesthesia machine for your practice.
Why Choosing the Right Anesthetic Machine Matters in Veterinary Practice
Anesthesia is not a one-size-fits-all process. Differences in patient size, species, and procedure type require equipment that can deliver precise, consistent control while adapting to a variety of clinical scenarios.
A well-matched machine supports accurate anesthetic delivery, effective ventilation, and safe pressure management, all while integrating smoothly into your team’s workflow.
For practice owners, it also plays a role in things like:
· Long-term reliability
· Maintenance costs
· Overall standard of care
Making it a foundational investment, not just another piece of equipment.
The Risks of Using Outdated Anesthetic Equipment in Veterinary Procedures
Using outdated anesthetic machines can introduce avoidable risks that impact both patient safety and clinical efficiency. Older equipment may lack modern safety features like:
Precise vaporizer calibration
Reliable pressure regulation
Effective leak detection
Increasing the likelihood of inconsistent anesthetic delivery.
Wear and degradation over time can also lead to equipment malfunction, gas leaks, or inaccurate monitoring, which could go unnoticed until they affect a procedure.
As standards of care continue to evolve, relying on aging equipment can make it more challenging to maintain predictable, controlled anesthesia across a wide range of patients and procedures.
A Practical, Streamlined Approach to Anesthesia
The Veta 3X is designed particularly for those working with limited space or lean teams. Its compact footprint allows it to integrate easily into existing treatment and surgical areas without extensive reconfiguration.
The system is intentionally straightforward, focusing on essential functionality like:
Consistent anesthetic delivery
Simple transitions between breathing systems
Clearly organized and accessible components
This design supports easy and efficient operation during procedures, especially in time-sensitive situations.
Built for Safety and Consistency
At the core of the Veta 3X is a fixed-mount isoflurane vaporizer with a pour-fill system, designed to deliver reliable anesthetic output. Key features that support patient safety include:
Adjustable APL valve for controlled pressure management
Visible and accessible breathing system components for monitoring
Integrated CO₂ absorber canister for effective gas management
These elements work together to promote consistent anesthetic depth and controlled delivery throughout procedures.
Designed for Everyday Veterinary Workflow
The Veta 3X incorporates design features that support daily use:
Organized hose and cable management to reduce clutter
Durable construction suited for high-use environments
Compatibility with both rebreathing and non-rebreathing systems
The included Bain system further supports flexibility, particularly for smaller patients requiring non-rebreathing anesthesia.
What’s Included
This configuration provides a complete anesthesia setup:
Fixed mount Iso vaporizer (pour fill)
O₂ hose
US gas hoses (DISS/DISS)
Bain system kit for Veta 3X
Disposable Bain circuit (1.2M)
These all work together, reducing the need for additional sourcing or compatibility concerns.
Cost and Warranty
The Veta 3X is available for $4,000, including shipping, and includes a 3-year parts-onlywarranty. This positions it as a practical option for:
New or expanding veterinary practices
Additional surgical suites
Facilities replacing older anesthesia equipment
The Mindray Veta 3X Anesthesia Machine offers a straightforward, reliable solution for veterinary anesthesia. Its design emphasizes essential functionality, ease of use, and compatibility with common clinical workflows, supporting consistent performance in a variety of practice settings.
The Warming Gap No One Talks About in Veterinary Surgery
Most veterinary teams don’t struggle with whether to keep patients warm—we all know it matters. The real challenge is consistency.
You can have all the right intentions, trained staff, and monitoring in place… and still end up with a patient whose temperature dips halfway through a procedure. Not because your team isn’t doing a good job, but because your warming setup isn’t working with you.
That’s the gap many veterinary hospitals are starting to notice, and it’s where theHoverHeatwarming blanket fits in.
The Reality of a Busy Surgery Day
Let’s zoom out for a second and look at a typical day in practice.
Back-to-back dentals. A couple of surgeries are running longer than expected. Different team members are rotating through anesthesia monitoring. Patients of all sizes, from a 5 lb cat to an 80 lb dog
In that environment, warming methods need to be simple, reliable, and low-maintenance.
Because if a system is cumbersome or inconsistent, it doesn’t reach its full potential. That’s where many traditional warming methods fall short. They often require constant adjusting, layering, or troubleshooting to stay effective.
Why Some Warming Setups Fall Apart Mid-Procedure
Even with multiple warming tools in place, temperature drops still happen. A few common reasons:
Heat isn’t reaching the areas that need it most
Warming is uneven or inconsistent
Setups shift during patient repositioning
Staff are too busy to continuously adjust equipment
In other words, it’s not just about having warmth; it’s about having dependable warmth that holds up throughout the entire case.
A More Practical Approach with HoverHeat
The HoverHeatwarming blanket was designed with real veterinary workflow in mind.
Instead of requiring constant attention, it provides a steady, even source of warmth that supports the patient without needing frequent adjustments.
Its underbody warming design helps address one of the most common breakdown points in temperature management—losing heat through prolonged contact with the surgical table.
For teams, that translates to:
Less time troubleshooting warming setups
Fewer last-minute “we need another blanket” moments
More consistent temperature trends on the monitor
And those small wins add up over the course of a full surgery day.
Especially Useful for Dental Days
If you’ve ever had a full dental schedule, you know how tricky temperature management can be. Dentals tend to involve:
Longer anesthetic periods than expected
Water exposure that contributes to heat loss
Frequent repositioning
Smaller patients who cool quickly
It’s the kind of setting where warming can easily become reactive instead of proactive.
Using a system like HoverHeat allows teams to build warming into the setup from the start, rather than chasing temperature drops later in the procedure.
Supporting Your Team (Not Just the Patient)
One overlooked benefit of a reliable veterinary patient warming system is how much it helps the team. When warming is predictable:
Anesthesia monitoring feels more controlled
Technicians can focus on trends instead of constant adjustments
There’s less mental load during already busy procedures
For former veterinary technicians, especially, this is a big deal. You know how many moving parts there are in anesthesia, and any tool that reduces friction is worth paying attention to.
Small Changes, Noticeable Differences
What makes the HoverHeatComplete Set appealing for many veterinary practices isn’t that it completely overhauls your workflow; it’s that it fits into it.
You’re not reinventing your surgery setup. You’re simply improving one piece of it in a way that’s:
Easy to implement
Simple to maintain
Consistent across different types of procedures
And over time, those small improvements show up in ways that matter, like with smoother recoveries, more stable anesthetic events, and less scrambling mid-procedure.
Where It Fits Into Your Current Setup
HoverHeatis designed to strengthen your approach to patient warming. It works alongside your existing protocols and equipment, helping create a more complete warming strategy for:
Surgery
Dentals
Recovery
Even longer or more complex cases
In real-world veterinary medicine, the goal isn’t perfection; it’s reliability.
You already understand the importance of keeping patients warm. But understanding it and achieving it consistently are two different things.
The HoverHeatwarming blanket helps close that gap by offering a practical, dependable solution that works with your team.
And when your warming system becomes one less thing to worry about, your entire surgical workflow benefits.
Preventing Hypothermia in Veterinary Patients: A Smarter Approach to Surgical Warming
Every veterinary team has experienced this:
You glance at the patient monitor halfway through a procedure and notice the body temperature slowly drifting downward. You add another towel, turn up the warm water blanket, maybe grab a heated air blanket—and still, keeping the patient warm can feel like an uphill battle.
Hypothermia during anesthesia is one of the most common challenges in veterinary surgery and dentistry. But with the right veterinary patient warming system, maintaining an ideal body temperature becomes far more manageable.
That’s exactly where the HoverHeat warming blanket is making a difference for veterinary hospitals.
Why Patient Warming Should Be a Priority in Veterinary Medicine
When your patient is under anesthesia, their body loses the ability to regulate temperature effectively. Combined with hair clipping, surgical prep, and exposure to a cool operating room, body heat begins to drop quickly.
That temperature drop matters more than many people realize. Anesthetic hypothermia can lead to:
Slower anesthetic recovery
Increased anesthetic complications
Delayed drug metabolism
Longer patient recovery times
In smaller patients, such as cats, puppies, or toy breeds, the temperature drop can occur even more quickly. That’s why many veterinary hospitals are investing in active warming systems designed specifically for veterinary surgical patients.
How the HoverHeat Warming Blanket Works
The HoverHeat veterinary warming blanket takes a different approach to temperature management than many traditional warming methods.
Instead of simply placing heat on the patient, the system uses a cushion of circulating warm air beneath the patient. This allows warm air to move evenly under the body, warming one of the largest heat-loss areas during surgery.
The result is more consistent heat distribution and improved patient warming throughout the procedure. For veterinary hospitals performing procedures like:
Routine spays and neuters
Dental procedures
Orthopedic surgeries
Soft tissue surgeries
…this type of active warming can make a noticeable difference in maintaining stable body temperatures.
Multiple Ways to Warm Patients
One advantage of the HoverHeat warming system for veterinary practices is its versatility.
The system can be used for:
Surgical Procedures: helping to maintain patient temperature throughout anesthesia, especially during longer procedures.
Veterinary Dental Procedures: dentals often involve extended anesthesia times and significant heat loss due to water exposure and patient positioning. Active warming helps keep temperatures stable during these cases.
Recovery: Patients recovering from anesthesia are often still prone to hypothermia. Maintaining warmth during recovery helps support smoother, more comfortable wake-ups.
Designed for Busy Veterinary Hospitals
Veterinary teams need equipment that works with their existing workflow, not something that adds extra complexity to surgery days. The HoverHeat is designed with practicality in mind.
Key features include:
Multiple pad sizes to accommodate different patient sizes
Compatibility with common warm air blowers already used in veterinary practices
Reusable design that reduces disposable blanket costs
Easy cleaning with standard hospital disinfectants
The ability to connect two units for additional warming coverage
For practices focused on improving veterinary surgical efficiency and patient safety, these small workflow improvements can make a big difference over time.
Supporting Better Surgical Outcomes
Veterinary medicine has advanced significantly in patient care standards, particularly in anesthesia monitoring and safety. Today, most hospitals routinely monitor:
ECG
Blood pressure
Oxygen saturation
End-tidal CO₂
Temperature
But monitoring temperature is only half the battle. Preventing hypothermia requires reliable warming tools that work throughout the entire procedure.
Using an active veterinary surgical warming system helps maintain stable patient temperatures from induction through recovery.
And when patients stay warm, everything tends to go more smoothly, from anesthesia recovery to overall patient comfort.
A Simple Upgrade That Makes a Big Difference
You’re always looking for ways to improve patient care while keeping procedures efficient and safe. Sometimes the biggest improvements come from solving everyday problems, like keeping anesthetized patients warm.
The HoverHeat warming blanket is a simple, reliable way to address one of the most common anesthesia challenges in veterinary medicine.
Because when patients stay warm, they recover better, and that’s something every veterinary team hopes for.
Keeping Veterinary Patients Warm with HoverHeat
With your experience in a veterinary surgery suite, you already know one thing for certain: anesthetized patients get cold, fast.
Whether you’re performing a routine spay, a dental cleaning, or an orthopedic procedure, maintaining normothermia isn’t just about comfort—it’s a critical part of patient safety and recovery. And yet, many veterinary hospitals still struggle to keep patients warm consistently throughout anesthesia and recovery.
That’s where patient-warming solutions like the HoverHeat are making a noticeable difference in veterinary practices.
Let’s take a closer look at why temperature management matters so much, and how systems like HoverHeat help veterinary teams stay ahead of the problem.
Why Veterinary Patients Get Cold During Procedures
Hypothermia during anesthesia is incredibly common in veterinary medicine. Even in short procedures like dentals, a patient’s body temperature can drop quickly.
There are several reasons for this:
Anesthesia suppresses thermoregulation. The body loses its ability to maintain temperature.
Hair clipping and surgical prep increase heat loss.
Exposure to cool surgical suites.
Contact with cold surgical tables.
Small body size, especially in cats and small dogs.
Most heat loss during surgery occurs at the point where the body contacts the table. That large surface area becomes a major pathway for conductive heat loss. When hypothermia sets in, it can lead to:
Slower anesthetic recovery
Increased anesthetic risk
Delayed drug metabolism
Longer hospitalization or recovery times
The Challenge With Traditional Warming Methods
Veterinary teams have historically relied on a mix of warming methods:
Circulating warm water blankets
Heated pads
Warmed IV fluids
Blankets and towels
Forced-air warming blankets
While these methods can help, many have limitations. Water blankets can leak. Heating pads can create hot spots. Disposable forced-air blankets can allow warm air to escape and require constant restocking. And most systems only warm one side of the patient.
That’s where the HoverHeat system takes a different approach.
How HoverHeat Works
The HoverHeat is a veterinary patient warming system designed to maximize heat transfer while minimizing the limitations of traditional warming tools.
Its design uses specialized internal components to create a cushion of warm air underneath the patient, effectively “levitating” the patient slightly while warm air flows beneath the body.
Why does this matter?
Instead of just heating the patient's top or small contact points, HoverHeat distributes warmth across a much larger area, helping maintain a more stable body temperature throughout the procedure.
Underbody and Overbody Warming
One of the most practical features for busy surgical suites is the ability to connect two HoverHeat units together.
With a simple connector, you can create simultaneous underbody and overbody warming with a single warm-air blower, increasing warming capacity by 50–75%. This means veterinary teams can:
Warm patients from below and above
Maintain temperature during longer procedures
Support smaller or high-risk patients more effectively
Importantly, the system is also designed so that airflow is directed away from the sterile surgical field, which helps maintain proper surgical protocol.
Warming Throughout the Entire Patient Journey
Another advantage is that it isn’t limited to the surgical table. It can be used during:
Pre-Operative Warming
Patients can be induced directly on the warming surface, allowing temperature management to begin immediately. Pre-operative warming has been shown to help maintain body temperature during surgery.
Intra-Operative Care
It works with most positioning devices and can be used during nearly any procedure, including surgery, dentistry, and endoscopy.
Post-Operative Recovery
Maintaining warmth during recovery can help decrease recovery times and improve patient comfort.
Imaging
Because of its design, the system can even be used during imaging procedures like X-ray and CT scans.
A Practical System for Veterinary Hospitals
For practice owners and managers, equipment decisions are always about balancing patient care, efficiency, and cost. HoverHeat addresses several practical concerns:
Compatible with existing warm air blowers: no need to purchase a new unit.
Reusable system: eliminates ongoing disposable blanket costs.
Easy to clean with standard germicidal sprays or soap and water.
Multiple sizes to accommodate patients from cats to large dogs.
The complete set includes small, medium, and large HoverHeat units plus connectors and adapters, allowing teams to warm nearly any patient that comes through the door.
Better Temperature Control, Better Patient Care
Every veterinary team member knows the feeling of watching a patient’s temperature drift downward during anesthesia. Preventing hypothermia can sometimes feel like a constant battle.
But with the right tools in place, maintaining normothermia becomes much easier and far more consistent. Because at the end of the day, a warm patient is a safer patient.
Stop the Beeping: Using ChatGPT and Gemini to Troubleshoot Veterinary Equipment
Picture this: The autoclave emits a piercing, rhythmic beep. Sterilization is backing up, surgery starts in 45 minutes, and your technicians are staring at the control panel like it just spoke in a forgotten language.
Inevitably, someone asks, “Should we call support?”
Maybe. But before you spend 40 minutes on hold or trigger a $250 service call fee, there is a better starting point. If you aren’t using animal hospital AI tools like ChatGPT or Gemini as your first troubleshooting step, you’re leaving time, money, and sanity on the table.
Why Veterinary Teams Need an "AI-First" Mentality
In a busy practice, equipment issues don’t just slow you down; they derail patient care. Traditionally, troubleshooting meant hunting for a 78-page PDF manual or watching a 14-minute YouTube video that—infuriatingly—features a slightly different model than yours.
By using AI-powered assistants, you get a "research shortcut" that:
Summarizes manuals: No more scrolling through hundreds of pages.
Cross-references data: Pulls from forums, manufacturer FAQs, and technical guides instantly.
Offers real-time refining: You can talk back to the AI to narrow down the specific symptoms you’re seeing.
The Secret Sauce: Writing Effective Prompts
The quality of the help you get depends on the quality of the "ask." Don't just say, "The autoclave is broken." Give the AI context.
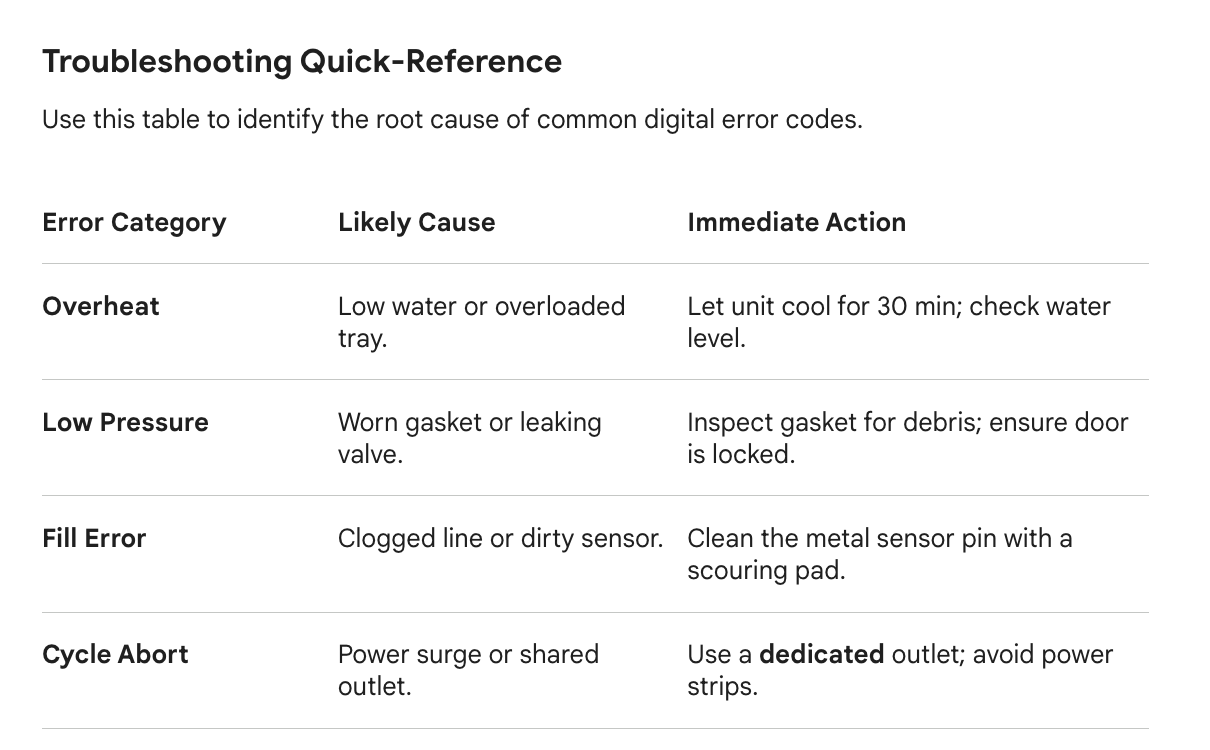
Option 1: Troubleshooting an Error Code
Effective Prompt: "I am a veterinary technician working with a Midmark M11 UltraClave. The screen is displaying Error Code E003. Can you provide a prioritized list of common causes for this code, and give me a step-by-step guide on how to perform the most likely basic fix (like cleaning the filters or checking the gasket)?"
Option 2: Solving a Performance Issue (ICU Cage)
Effective Prompt: "Our Snyder ICU Oxygen Cage is struggling to maintain humidity levels above 40%, even though the reservoir is full. Act as a biomedical repair expert. What are three specific mechanical components I should check for clogs or leaks before I call a professional technician?"
A three-Step Workflow for Your Team
To turn this into a hospital-wide habit, implement this "AI-First" Equipment Protocol:
Step 1: The Specific Query
Instead of a vague search, feed the AI the Brand, Model, and specific symptom. * Tip: If you are using the mobile app, you can even take a photo of the error screen (with ChatGPT Plus or Gemini Advanced) and ask, "What does this error message mean?"
Step 2: The "Safety First" Follow-Up
Once the AI suggests a fix, ask: "Are there any safety risks associated with checking the [Component Name], and will opening this panel void our manufacturer's warranty?" This keeps your team safe and your equipment protected.
Step 3: Document the Attempt
If the AI fix works, have the tech copy the steps into your practice management software or a "Troubleshooting Log." If it doesn't work and you still have to call support, you can now tell the technician exactly what you’ve already tried, which often speeds up their diagnostic time.
The ROI: Why Practice Owners Should Care
Every unnecessary service call has a "hidden" cost:
Direct Fees: Travel fees and hourly labor.
Opportunity Cost: Canceled surgeries or delayed diagnostics.
Team Morale: Technicians feel empowered when they can solve a problem themselves rather than waiting for "the expert" to show up.
A Word of Caution: AI is a brilliant research assistant, not a licensed repairman. Never attempt to bypass safety sensors, disassemble pressurized chambers, or perform electrical work beyond basic fuse replacement unless you are qualified.
Try This Tomorrow
The next time a piece of equipment acts up—whether it's a finicky blood chemistry analyzer or a jammed paper shredder—don't reach for the phone first. Open ChatGPT or Gemini, input the model number, and describe the problem.
Stop the Blur: Using Gemini AI to Master Large-Dog Radiographs
You position beautifully. You center carefully. You collimate appropriately. You hit expose…
And the image comes up blurry. Not just “a little soft,” but diagnostically questionable.
Full-body radiographs on 100lb Labs or obese cats can humble even the most experienced teams. When you’re up against thickness, motion, scatter, and time pressure, things get tricky fast. This is where Gemini, Google’s AI collaborator, becomes an essential tool for your radiology suite.
Sometimes you don’t need more CE; you need a fast, clear answer while the patient is still on the table.
Step 1: Moving Beyond Generic Search
If your team types: “Why are my x-rays blurry?” they’ll get a generic article. To get "Level 2" results, teach your staff to use Power Prompts that include specific constraints and a requested format.
The Power Prompt: "Act as a senior veterinary radiographer. Give me a 4-point checklist to fix motion blur for a 95lb dog on a DR system. Focus only on kVp/mA adjustments and physical restraint. Keep it under 50 words."
Step 2: Troubleshooting with "Physics-to-Practice"
Most of us don't need a physics lecture mid-shift. We need reminders that translate to immediate action. Instead of asking "why" something works, ask Gemini how to apply it to your specific machine.
The Power Prompt: "I’m shooting a 100lb dog, and the image is blurry from respiratory motion. My current settings are [Insert Your Settings]. What specific mA increase and exposure time decrease do you recommend to stop motion while maintaining density?"
Step 3: Create Instant Clinical "Cheat Sheets"
If your team struggles with consistency, use Gemini to build a reference tool that can be printed and taped to the wall near the generator.
The Power Prompt: "Create a simplified technique chart table for 'Large/Obese Patients' on a DR system. Include columns for: Body Thickness (cm), Grid Use (Yes/No), and kVp adjustment factors. Format it as a clean, scannable table."
Step 4: Mastering Motion Control
Blurry images aren’t always about the settings; they’re about the patient. Gemini can help your team refine their physical approach in seconds.
The Power Prompt: "List the 3 best sedation protocols and 2 positioning aids specifically for reducing respiratory motion in obese cats during thoracic films. Bullet points only."
Why This Matters for Your Workflow
A blurry radiograph is more than just a bad image; it’s a drain on your practice's health. Retakes lead to:
Increased Radiation: Unnecessary exposure for staff and patients.
Bottlenecks: A 10-minute study turning into a 30-minute ordeal.
Staff Burnout: Frustration from "guessing" at settings.
3 Tips for "Talking" to Gemini in the Clinic
Assign a Persona: Start your prompt with "Act as a senior veterinary radiographer" to ensure a professional tone and clinically grounded advice.
Use Specific Constraints: Tell the AI to "Keep it under 50 words" or "Use bullet points." This prevents you from having to read a long article while a patient is on the table.
Give It Your "Inputs": If you want a better setting, tell Gemini what you are currently using. AI is best at suggesting the "next step" when it knows where you are starting.
The "Why" Behind the Prompt
Using Gemini proactively reduces retakes, minimizes staff frustration, and ensures diagnostic-quality images the first time—improving both patient care and clinic efficiency.
The Bottom Line: AI as a Clinical Confidence Tool
We tend to talk about AI as if it’s only for "robotic" diagnostics. But in a busy clinic, Gemini’s best use is helping a technician stand in front of a DR monitor, think clearly, and get the shot right the second time—or better yet, the first.
Why AI Works:
AI answers improve dramatically when it knows:
What equipment
What happened
What you observed
What help do you want?
Think of it like calling tech support — details matter.
How Veterinary Teams Can Use ChatGPT as a Troubleshooting Partner for In-House Lab Analyzers
If you’ve ever been in the middle of a packed schedule, samples piling up, and your in-house analyzer suddenly throws an error code that looks more like a license plate number than helpful information… you’re not alone.
Most veterinary hospitals rely heavily on in-house lab analyzers and other equipment from IDEXX, Heska, and Abaxis. These analyzers are incredible tools, but when something goes wrong, the immediate reflex is often: “Ugh. Who’s calling support this time?”
Here’s a handy little secret: many of those calls are avoidable.
Let’s peek behind the curtain of animal hospital AI, specifically tools like ChatGPT, and the growing role of veterinary AI inside modern practices.
Used correctly, ChatGPT can act like a calm, knowledgeable partner for your team, helping to interpret error codes, think through next steps, and often resolve issues before you ever pick up the phone.
Let’s talk about how…
First, a mindset shift: ChatGPT isn’t replacing support, it’s triage
Important disclaimer upfront: ChatGPT isn’t a substitute for IDEXX, Heska, or Abaxis support. But it is an incredibly useful first line of troubleshooting.
Think of veterinary AI like this:
It helps you understand what the error likely means
It helps you rule out common causes
And when you do call support, you’re far more prepared
That alone can save time and frustration.
Let’s break it down…
Step 1: Feed ChatGPT the right information
Veterinary AI is only as good as the details you give it. When an error pops up, avoid typing something vague like “My oxygen concentrator has an error.” Instead, input specifics.
True story: Lilli, a seasoned veterinary team member from Baker Vet Services, reached out recently.
“I have a question that we were wondering if you could help with. Our oxygen concentrator shows a power failure, but the cord is fine. Is there anything you can do to try to fix it? We’ve checked the cord, filters, and outlets.”
After some encouragement to enter the problem, make, and model number into ChatGPT, Lilli was relieved to discover it was the fuse causing the trouble and was able to quickly get it fixed.
Step 2: Ask ChatGPT to explain the error like you’re a tech on the floor
One of the biggest advantages of veterinary AI is its translation capabilities. Manufacturer manuals are thorough… but not always quick to interpret in the middle of a busy day.
Try prompts like:
“Explain this Abaxis VetScan error code in simple terms.”
“What does this Heska analyzer error usually indicate during sample processing?”
“What are the most common reasons this IDEXX error occurs?”
ChatGPT won’t just repeat the error; it will often explain why it happens, which is key for preventing repeat issues.
Step 3: Use veterinary AI to create a step-by-step troubleshooting checklist
This is where things get really powerful for hospital operations.
Ask ChatGPT: “Create a step-by-step troubleshooting checklist for this error, starting with the most common and least invasive fixes.”
For example, veterinary AI might suggest:
Checking reagent expiration dates
Inspecting sample volume and quality
Running a clean cycle
Power cycling the analyzer properly
Many of these are things experienced technicians already know—but in the moment, stress can cloud logic. Animal hospital AI helps slow things down and bring clarity.
Step 4: Ask how to prevent the error from happening again
This is the step most teams skip. Once the issue is resolved, ask:
“What maintenance steps help prevent this error in the future?”
“Is this error commonly caused by user technique, environment, or consumables?”
“What daily or weekly checks reduce the likelihood of this happening again?”
Over time, this turns ChatGPT into a training assistant, not just a troubleshooting tool.
Step 5: Document smarter (and faster)
Here’s an underrated benefit: veterinary AI can help your team document issues clearly.
What ChatGPT should not be used for.
Veterinary AI has limits. Your team should still call support when:
The analyzer instructs you to stop use immediately
There’s a repeated mechanical failure
Patient safety could be compromised
Animal hospital AI is a guide, not a green light to override manufacturer safety protocols.
Why this matters for practice owners
For veterinarians and practice owners, this isn’t just about convenience. Using veterinary AI effectively can:
Reduce analyzer downtime
Minimize unnecessary support calls
Decrease frustration
And most importantly, it helps your team feel supported, even when things go sideways.
Veterinary AI as a partner in crime
Animal hospital AI isn’t replacing people; it’s simply giving smart, capable teams better tools to think, troubleshoot, and move forward with confidence. Anything that helps a tech avoid standing on hold while samples stack up is a win in anyone’s book.
The opportunity is sitting right in front of you. It just needs to be used intentionally.
Because sometimes, the fastest support line is the one already in your pocket.
Veterinary Autoclave Troubleshooting Guide
In the fast-paced environment of a veterinary clinic, the autoclave is the unsung hero. When it works, surgical packs are sterile and ready for the next spay or dental. When it doesn't? Your entire schedule grinds to a halt.
Here is a guide to the most common autoclave headaches and how to fix them before they disrupt your day.
1. The Temperature Just Won’t Rise
If your unit is stuck in a preheat loop or isn’t hitting the required 121°C (250°F), you aren’t just losing time—you’re compromising sterility.
The Culprit: Often, this is a water level issue. If the reservoir is low, the heating element can't generate enough steam.
Check This: Ensure you are using distilled water only. Tap water can cause mineral buildup (scale) on heating elements, acting as insulation that prevents heat transfer.
The Fix: Clean the heating element with a specialized autoclave cleaner and ensure the water sensor is free of debris.
2. The Infamous "Wet Pack."
You open the door, and the surgical wraps are damp. In the veterinary world, a wet pack is one that is contaminated.
The Culprit: This is usually a loading error. If packs are stacked too tightly or "nestled" together, steam can't circulate, and moisture gets trapped.
Check This: Is your chamber filter clogged? If the air-jet or drain filter is blocked with lint or hair (a common vet clinic reality!), the vacuum/drying phase will fail.
The Fix: Use a rack to separate pouches. Ensure paper-plastic pouches are placed on their sides (like files in a folder) rather than flat.
3. Steam Leaking from the Door
If you hear a "hissing" sound or see steam escaping around the front of the machine, your cycle will likely fail due to pressure loss.
The Culprit: The door gasket (the rubber ring) is likely worn, dry, or dirty.
Check This: Look for small cracks or bits of surgical tape stuck to the gasket. Even a tiny piece of debris can break the seal.
The Fix: Wipe the gasket daily with a damp, lint-free cloth. If it’s cracked, it’s time to order a replacement.
4. "Error Code XXX."
Modern autoclaves are smart—sometimes too smart. They’ll throw a code like "E001" or "Cycle Aborted" and refuse to move.
The Culprit: This could be anything from a power surge to a faulty solenoid valve.
The Fix: Don’t guess. Every brand has a specific "Error Code Table." Below, I’ve provided a way to get the answer instantly.
The Autoclave "Power Prompt"
If your autoclave is acting up and the manual is nowhere to be found, use this prompt with an AI assistant to get a specialized diagnosis.
Copy and paste the text below, filling in the bracketed information:
"I am a veterinary professional troubleshooting an autoclave. The brand is [Insert Brand, e.g., Midmark, Tuttnauer, Ritz] and the model is [Insert Model Number].
The specific issue I am seeing is: [Describe the problem, e.g., Error Code E007 / Water leaking from bottom / Cycle won't start].
Based on the manufacturer’s service manual for this specific model, can you tell me:
What are the most likely causes for this specific error?
What are the 'first-step' fixes I can do in the clinic?
At what point do I need to stop and call a professional technician?"
Pro-Tip: The "Golden Rule" of Autoclaves
90% of autoclave failures in vet clinics are caused by two things: Poor water quality and hair/lint buildup. A weekly cleaning routine can save you thousands in repair bills.
Since many autoclave issues in a veterinary clinic stem from hair, dander, and mineral buildup, a consistent maintenance schedule is the best defense.
Here is a printable-style Weekly Maintenance Checklist you can post in your sterilization area.
🏥 Veterinary Autoclave: Weekly Maintenance Checklist
Goal: Prevent "Error Codes," "Wet Packs," and heating element failure.
✅ Monday: The Deep Clean
Drain the Reservoir: Empty all water from the reservoir. Stagnant water grows biofilm and concentrates minerals.
Chamber Scrub: Use a non-chlorinated, manufacturer-approved cleaner (like Omni-Cleaner or Speed-Clean). Scrub the bottom of the chamber to remove any "cooked-on" debris or surgical tape residue.
Rinse & Refill: Rinse the chamber thoroughly with distilled water and refill the reservoir to the "Full" line.
✅ Wednesday: The "Seal & Filter" Check
Gasket Inspection: Wipe the door gasket with a damp, lint-free cloth. Look for cracks, pits, or any pet hair that might break the vacuum seal.
Clean the Chamber Filter: Locate the small mesh filter at the bottom or back of the chamber. Remove it and rinse away any lint or hair.
Tip: If this is clogged, your packs will stay wet!
✅ Friday: The Performance Test
Biological Indicator (BI) Test: Run a spore test to ensure the autoclave is actually killing microorganisms, not just getting hot. Log the results in your clinic’s sterilization binder.
Tray & Rack Check: Remove the trays and the wire rack. Wipe them down to prevent oxidation (rust) from forming, which can transfer to your stainless steel instruments.
🚫 The "Never" List (Post this for new staff!)
NEVER use tap water. It will ruin the heating elements within weeks.
NEVER use steel wool or wire brushes to clean the chamber (it causes pitting and rust).
NEVER overload the trays. If steam can't circulate, the center of the pack isn't sterile.
Since different brands use different codes (for example, a "C-001" on one machine might be an "E-003" on another), I’ve designed this Troubleshooting Quick-Reference by "Error Type."
This makes it easy for your staff to identify the root cause based on what the machine is doing or saying.
⚡ Autoclave Troubleshooting Quick-Reference
Keep this near the autoclave for immediate diagnosis.
Common Error Categories
Error Type
Common Codes (Varies)
Probable Cause
Immediate Action
Overheat
E001, E1, Hi-Temp
Low water, overloaded chamber, or faulty sensor.
Vent steam, let the unit cool for 30 min, and check the water level.
Low Pressure
E002, P-Low, Vac-Fail
Worn door gasket or leaking safety valve.
Inspect the gasket for debris; ensure the door is locked tight.
Fill Error
E003, No-Water
Clogged water line or dirty water sensor.
Clean the sensor (the small metal pin) with a scouring pad.
Cycle Abort
E007, Power-Fail
Power surge or unstable voltage.
Plug the unit into a dedicated outlet (no power strips!).
Dry Failure
Wet Pack, E009
Clogged chamber filter or poor loading.
Clean the filter mesh; reload packs on their sides.
The "3-Step Rescue" Protocol
If an error occurs mid-cycle, follow these steps immediately:
Safety First: Do not attempt to force the door open if the pressure gauge is above zero.
The "Hard Reset": Many software glitches can be cleared by turning the power switch OFF for 60 seconds and then back ON.
Check the "Big Three":
Is it Distilled Water?
Is the Gasket clean?
Is the Filter clear of hair/lint?
When to Call for Service 📞
If you see these "Red Flag" issues, stop using the machine and call a technician:
Burning smell: Indicates a short circuit or a fried heating element.
Constant Hissing: Even after cleaning the gasket, steam continues to escape.
Water Under the Unit: A sign of a blown internal hose or a failing weld.
Customizing This for Your Clinic
To make this perfectly accurate for your team, you can look up the "Error Code Table" in your manual and jot down the most common ones here:
Code ______: Meaning: ____________________________________
Code ______: Meaning: ____________________________________
Why Cat-Specific Cages Matter in Rescue Facilities (More Than You Might Think)
The goal of a cat rescue isn’t just to provide a home for these furry creatures; it’s to help them heal, decompress, and to help them get adopted by a loving family.
Rescue environments are full of good intentions and hard realities, such as limited space, high intake, unknown medical histories, and cats arriving stressed, scared, or shut down. In that setting, the type of cage system you use can quietly make—or break—everything that follows.
Cat-specific cage systems give cats the best possible chance to recover, socialize, and move on to a permanent home.
Stress Is Often the Biggest Barrier to Adoption
Many rescued cats don’t show their true personalities right away. Instead, stress takes over.
You see it as:
Hiding in the back of the cage
Refusing food
Aggression or shutdown behavior
Over-grooming or stress-induced illness
When cats are confined in cages not designed for feline behavior, stress compounds quickly. Loud noises, lack of vertical space, no separation between litter, food, and resting areas—it all sends the same message to the cat: “You’re not safe here.”
A cat-specific cage system helps change that narrative.
Cats are territorial and routine-driven animals. When a cage respects those instincts, cats settle faster. Cat-specific systems typically allow for:
Separate zones for litter, food, and rest
Vertical space so cats can perch or retreat upward
Visual barriers to reduce overstimulation
Easy-to-clean surfaces that minimize lingering stress pheromones
These design elements reduce cortisol levels, which directly impacts appetite, immune function, behavior, and sociability.
Recovery and Behavioral Assessment All Improve
Rescue facilities juggle multiple stages of care at once:
Intake and quarantine
Medical treatment or recovery
Behavioral observation
Adoption readiness
Cat-specific cage systems make it easier to do things like:
Monitor eating, litter use, and demeanor
Perform daily care without escalating fear
Identify real behavioral issues versus stress responses
When cats aren’t constantly in survival mode, staff and volunteers get a more accurate picture of who that cat really is. Allowing their personality to really shine through.
Better Cages Support the Humans, Too
Rescue work is emotionally and physically demanding. Cat cages not only benefit those being housed in them, but also those who are maintaining that space by:
Reducing the risk of bites and scratches
Allowing for easier spot-cleaning and full sanitation
Improving workflow during feeding and medication rounds
Making daily care less stressful for staff and volunteers
When cats are calmer, the people caring for them feel the difference, too.
Adoption Outcomes Improve
Potential adopters are drawn to cats who:
Are visible and relaxed
Show curiosity or social interest
Aren’t crouched in fear at the back of the cage
A cat cage system helps cats present their best selves. It doesn’t change who they are—it simply removes the barriers that keep their personalities hidden. That leads to:
Shorter length of stay
Higher adoption rates
Better matches between cats and adopters
It’s Really About Compassion, Not Perfection
No rescue has unlimited resources. And no cage system can fix everything.
But choosing a cage system designed specifically for cats sends a powerful message to the animals, your team, and your supporters: “We understand cats, and we’ve built our care around them.”
That intention alone can transform a rescue space from a holding area into a place of healing.
In rescue work, every small improvement matters. And few changes have as wide-reaching an impact as giving cats a space that truly meets their needs.